Positioning MRI as an Effective Prostate Cancer Screening Tool
Study shows that MRI helped detect more clinically significant disease without biopsy

Often exhibiting no symptoms until an advanced stage, prostate cancer remains a difficult disease to detect. While screening can help, current practices, which test for prostate-specific antigen (PSA) levels, lack specificity and can be elevated for reasons other than cancer. MRI has the potential to close this screening gap.
“MRI can help differentiate more aggressive, clinically significant cancers and guide biopsy and treatment,” said Carla Harmath, MD, associate professor of radiology at University of Chicago Medicine.
Benefits And Challenges of Imaging Prostate Cancer
When it comes to prostate cancer, MRI is already being used to explore differences in proton physics and water diffusion in cancer tissue compared to the normal gland, with the differences producing a specific appearance to the normal background glandular tissue.
Furthermore, thanks to the evolution of higher resolution images, along with multiparametric (mpMRI) evaluation of the gland, MRI can now detect clinically significant prostate cancer with higher sensitivity and specificity than ever before.
Yet despite this screening potential, challenges remain.
“When developing a screening tool, we want it to be available for the population in general, and MRI is still a costly exam and one not readily available in many health care systems,” explained Dr. Harmath, who authored a Radiology editorial on the topic.
Prostate MRI exams can also be very challenging to interpret. For example, several non-cancerous abnormalities of the prostate gland such as inflammation can provide a similar MRI appearance to cancer, promoting false positive findings, while other cancers are not well visualized, promoting false negative findings.
“The subjectivity and variability in interpretation can impact the accuracy of the diagnosis,” Dr. Harmath added.
Another key challenge is variability in image quality, which, as Dr. Harmath explained, can suffer due to alterations in the patient’s anatomy, body habitus or the presence of bowel gas.
“Since the diagnosis relies heavily on the apparent diffusion coefficient map, which is very susceptible to artifacts, mild differences can become major artifacts on the images,” she said.
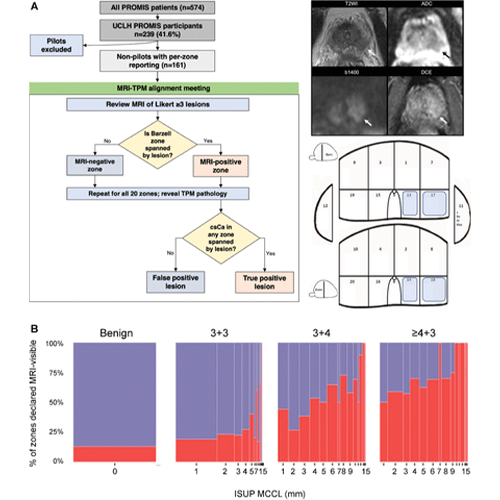
(A) Flowchart shows participant population and MRI–transperineal mapping (TPM) alignment. The study included 161 nonpilot Prostate MRI Imaging Study (PROMIS) participants from University College London Hospitals (UCLH) who underwent multiparametric MRI followed by a combined biopsy procedure and detailed per-zone recording of Gleason grade and maximum cancer core length (MCCL) per the International Society of Urological Pathology (ISUP) definition. A consensus multidisciplinary panel, blinded to TPM findings, reviewed MRI scans and aligned any lesions with a Likert score greater than or equal to 3 to specific Barzell zones before the pathologic status was revealed. For example, the left peripheral zone lesion shown on the right was aligned to zones 13,14,17, and 18. (B) Spineplots show the percentage of zones deemed visible at MRI according to the overall Gleason score at TPM. The consensus panel determined the MRI positivity of 3179 zones; this was slightly less than the expected 3220 (161 participants × 20 zones) due to small prostate size in five men, which prevented full sampling of all Barzell zones. Of 3179 zones, 2516 were benign and, of those with cancer, 301 had a Gleason score of 3+3, 271 had a Gleason score of 3+4, and 91 had a Gleason score greater than or equal to 4+3. In total, 595 zones were MRI-positive (18.7%), although the proportion that were MRI-visible rose with increasing Gleason grade and with each additional millimeter of MCCL, motivating a zonal pathologic finding–based model of MRI positivity. ADC = apparent diffusion coefficient, b1400 = b value of 1400, csCa = clinically significant cancer, DCE = dynamic contrast-enhanced, T2WI = T2-weighted imaging. https://doi.org/10.1148/radiol.220762 ©RSNA 2022
The Relationship of the Gleason Grade to MRI Visibility
To address some of these challenges and advance MRI’s use as a screening tool, a Radiology study investigated the way prostate cancer grade and maximum cancer core length (MCCL) on transperineal mapping (TPM) biopsy impact the odds of an MRI lesion appearing within the biopsied prostate area.
“We know there is a correlation between specific MRI prostate signal intensity characteristics and the presence of clinically significant prostate cancer, yet there are few reliable numerical estimates of this association, especially in biopsy-naïve men with unperturbed prostates and a raised PSA,” said Vasilis Stavrinides, MD PhD, a clinical research fellow at the University College London Cancer Institute and the study’s lead author.
The research builds on the PROMIS study, during which men with raised PSA underwent MRI followed by a biopsy, regardless of imaging findings and whether a lesion was present.
In the Radiology study, PROMIS participants underwent extensive 5-mm TPM biopsies of their entire prostate, with their pathology reported both at the whole-organ level and for each of 20 standard prostate zones.
Researchers investigated the relationship between Barzell zone pathologic findings (Barzell being a technique by which the prostate is divided into an eight-sector template divided by three planes) and the odds of that same zone being declared MRI-visible by a team of expert clinicians.
Doing so allowed researchers to derive 20 binary outcomes per patient—one for each zone. It also meant they could use a statistical method called a generalized mixed model to predict outcomes using zonal Gleason, a system for grading how abnormal prostate cancer cells look and how likely the cancer is to advance and spread, and MCCL as explanatory variables.
“We showed that, on average, Gleason 3+4 disease increased the odds of a prostate area being visible on MRI by a factor of three, whereas high-grade prostate cancer—Gleason 4+3 or higher—increased the odds by almost nine times,” Dr. Stavrinides said.
The study repeated this same process in TPM-negative men, this time using the presence of prostatic intraepithelial neoplasia (PIN), inflammation or atypia as predictors. In this scenario, the presence of PIN was the major determining factor of false positive lesions in men without cancer on TPM.
Reiterating MRI’s Advantage
Based on these findings, the research team developed a model showing how MRI lesions in the prostate are determined by prostate cancer aggressiveness and cancer extent. “This model demonstrated how low-grade, low-volume disease is typically not represented on MRI, reiterating that MRI’s advantage is its ability to disregard insignificant disease while readily detecting clinically important tumors,” Dr. Stavrinides noted.
The team also provided statistical estimates of the association between tissue and imaging—estimates that could play a big role in developing new imaging approaches for detecting prostate cancer. “This research confirms that we are moving in the right direction in terms of working with MRI as a potential screening tool,” Dr. Harmath said. “Furthermore, it opens the door to technological advances that could increase the sensitivity and specificity of this imaging modality in the diagnosis of prostate cancer.”
For More Information
Access the Radiology study, “Regional Histopathology and Prostate MRI Positivity: A Secondary Analysis of the PROMIS Trial” and the commentary, “Prospective Validation of MRI Signal Abnormalities and Clinically Significant Cancer.”
Read previous RSNA News stories on prostate cancer: