US Performs Comparably with MR Imaging for Quantifying Fatty Liver Disease in Children
Imaging can be used to rule out other causes of liver disease




Metabolic dysfunction-associated steatotic liver disease (MASLD)—formerly known as Non-Alcoholic Fatty Liver Disease (NAFLD) – is on the rise in young patients. A prospective study suggests that ultrasound (US) stacks up well to MR imaging for diagnosing MASLD, giving clinicians and families more options.
“Ultrasound is more widely available than MR imaging, in part due to a lower equipment cost,” observed study senior author Andrew Trout, MD, director of clinical research and professor of radiology at Cincinnati Children’s Hospital Medical Center. “Knowing that both ultrasound and MR quantitative measures of liver disease agree reasonably well means that either technique can be used with good diagnostic performance.”
In a separate NIH study, published in Clinical Liver Disease, investigators found that MASLD has become common in children, with a prevalence as high as 10% in some populations. It’s most common in older children and males—one of the strongest risk factors being obesity.
Correlations Between US and MRI Measures of Stiffness and of Liver Fat
“Most quantitative imaging techniques are developed with adults in mind and validated in adult populations,” Dr. Trout pointed out, so his team aimed to specifically evaluate the performance of quantitative US techniques in pediatric patients. They recruited 44 participants between the ages of 8 and 21 years with known or suspected MASLD. Patients were imaged with both US and MRI using techniques to quantify liver fat content and liver stiffness which is a marker of fibrosis that can develop in more advanced MASLD.
In their study, published in Radiology, the researchers found positive correlation between US shear-wave speed and stiffness measured on MR elastography. In terms of predicting abnormal liver shear stiffness, US yielded an area under the receiver operating curve of 0.95, with 91% sensitivity and 95% specificity. When it came to predicting abnormal liver fat, attenuation on US was moderately useful as well, showing 73% sensitivity and 73% specificity when compared with proton density fat fraction MR imaging.
The authors concluded that both US and MR imaging are reasonable alternative methods to noninvasively quantify liver disease—in children with a body mass index less than 35 kg/m2. One limitation of the study was that no children had a body mass index above 35 kg/m2.
“The majority of children with MASLD have risk factors like obesity but exhibit no symptoms. Based on the 2017 guideline by the North American Society for Pediatric Gastroenterology, Hepatology and Nutrition, screening for MASLD is advised for all children aged 9 to 11 years with obesity (body mass index ≥95th percentile) and for children who are overweight (body mass index ≥85th percentile) and have other risk factors like diabetes or family history,” said Vinicius Alves, MD, first author on the study, former research fellow at Cincinnati Children’s Hospital Department of Radiology and current first-year resident at Northwestern Medicine, Chicago. “In the past, this screening involved a blood draw to test serum alanine aminotransferase (ALT) levels as a marker of liver inflammation. The latest MASLD criterion, however, focuses on imaging or biopsy evidence of steatosis, though updated screening guidelines are yet to be released.”
US is often the first imaging test performed in patients with suspected MASLD. A child presenting with typical clinical features, such as obesity or cardiometabolic risk factors like diabetes or dyslipidemia and evidence of steatosis by imaging or biopsy can be diagnosed with MASLD once other potential causes of liver disease are ruled out.
Increased availability of quantitative diagnostic imaging techniques will allow radiologists to better diagnose MASLD, assess the severity of steatosis and fibrosis and to monitor progression over time, according to Dr. Alves.
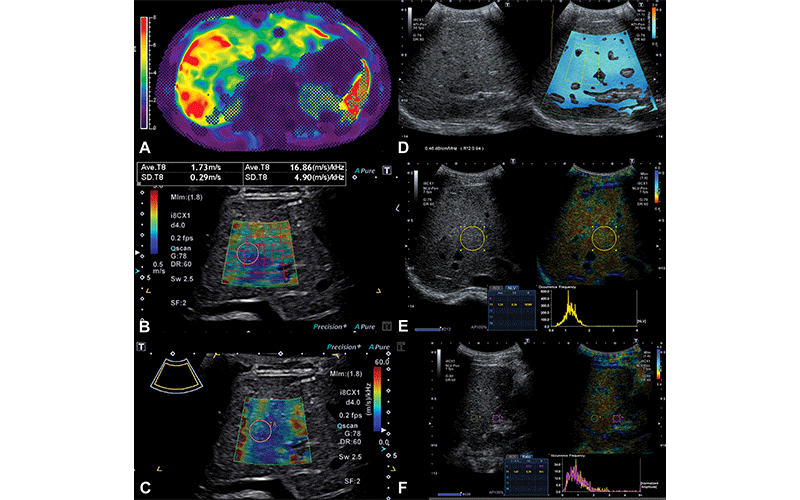
Representative MR elastography and quantitative US images in a 16-year-old boy with Fontan-associated liver disease and elevated liver shear stiffness (5.4 kPa with gradient-recalled echo MR elastography). (A) Axial MR elastogram with 95% confidence map overlay shows a stiff (5.4 kPa) heterogeneous liver. Image colors are indicative of stiffness (in kilopascals) according to the scale in the left of the elastogram image. (B) Transverse two-dimensional shear-wave elastography US image with shear-wave speed of 1.73 m/sec (9.0 kPa). (C) Transverse shear-wave dispersion map with dispersion of 16.86 m/sec/kHz. (D) Split-screen transverse image shows liver attenuation measurement of 0.46 dB/cm/MHz. (E) Split-screen transverse image shows normalized local variance measurement of 1.24. (F) Split-screen longitudinal image shows hepatorenal index measurement of 1.07. ATI-Pen = attenuation imaging penetration mode frequency, DR = dynamic range, fps = frames per second, G = gain, i8CX1 = Canon Apio i8CX1 transducer, Ml = mechanical index, NLV-Pen = normalized local variance penetration mode frequency, SF = spatial filter, Sw = shear-wave frequency. https://doi.org/10.1148/radiol.212995 ©RSNA 2022
Incorporating US Assessment of Hepatic Fat for Clinical Care
In an accompanying Radiology editorial, Geetika Khanna, MD, MS, and Adina L. Alazraki, MD, both from Children’s Healthcare of Atlanta and Emory University commented that “although obesity has not been shown to affect MR elastography, it remains a limitation for ultrasound. This is because the thickened subcutaneous tissue leads to sound attenuation, which limits the induction and propagation of shear waves through the tissues.”
Considering that a large proportion of children with hepatic steatosis have a BMI greater than 35 kg/m2, this limitation is particularly relevant, noted Drs. Khanna and Alazraki.
“Further studies are urgently needed for multivendor validation of quantitative ultrasound assessment of hepatic fat in the pediatric population so that these techniques can be incorporated into the clinical care of these patients,” they said.
The editorial authors pointed out that disruption of kids’ daily activities during the COVID-19 pandemic has worsened the incidence of pediatric obesity—children who were overweight before lockdown showed significantly higher rates of BMI increase over the course of the pandemic.
“A comprehensive imaging study that can provide a one-stop robust assessment of hepatic steatosis, inflammation and fibrosis in a cost-effective and child-friendly manner would favorably impact the follow-up of children with NAFLD and nonalcoholic steatohepatitis,” Drs. Khanna and Alazraki added.
Meanwhile, for children who can benefit from US evaluation, Dr. Trout’s team suggests that it’s a viable method—and could mean that more patients have access to quantitative noninvasive evaluation in areas where MR equipment is scarce.
“The quantitative techniques evaluated in this study provide an opportunity both to refine and facilitate diagnosis of an increasingly prevalent disease. The techniques are available across most vendor platforms, can be applied to both inpatients and outpatients, and can be accomplished without patient sedation,” Dr. Trout concluded. “Our results open the door to less invasive diagnosis techniques in children and young adults with obesity and who are overweight. It’s simply a matter of applying these techniques more widely.”
For More Information
Access the Radiology study, “Comparison of Quantitative Live US and MRI in Patients with Liver Disease,” at RSNA.org/Radiology.
Access the Clinical Liver Disease study at journals.lww.com/cld.
Information about fatty liver disease that is intended for patients can be found at RadiologyInfo.org.
Read previous RSNA News stories on liver imaging: