What Radiologists Need to Know About Post-Treatment Head and Neck Imaging
Imaging can help detect complications and disease recurrence

It can be particularly challenging to interpret post-treatment imaging in patients with head and neck cancer due to changes in tissue from treatment such as surgery, radiation, chemotherapy and immunotherapy. Radiologists need to understand these changes and how they appear on imaging to help differentiate between treatment-related changes and tumor recurrence.
“As radiologists, we see what others on the multidisciplinary team cannot see with direct visual inspection. Our role in the post-treatment setting is to distinguish expected findings from unexpected complications and detect recurrence early,” said Alok A. Bhatt, MD, professor of radiology at the Mayo Clinic in Jacksonville, FL, and senior author of a Radiology: Imaging Cancer article on this topic.
The article noted the common post-treatment findings seen on imaging and some unfamiliar entities such as hypertrophied superior cervical ganglia, inflamed thyroglossal duct cyst and immunotherapy-related adverse events, which should not be mistaken for disease recurrence.
“It is important to share this knowledge with radiologists, thus allowing us to provide guidance to health care teams and assist with patient care,” Dr. Bhatt said.
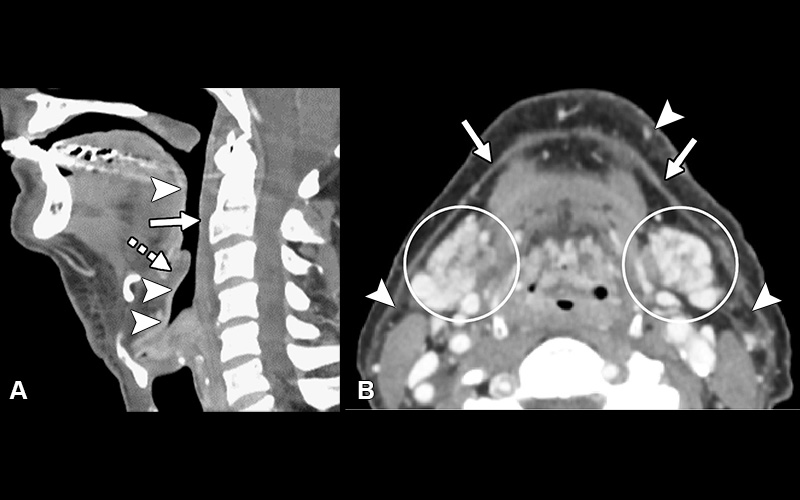
Postradiation-related changes—acute findings. (A) Sagittal postcontrast CT image demonstrates retropharyngeal edema (solid arrow), laryngeal mucoid edema (dashed arrow), and intense linear mucosal enhancement (arrowheads). (B) Axial postcontrast image demonstrates edema and intense enhancement of the submandibular glands (circled), thickening of the platysma muscle (arrows), and stranding of the fat (arrowheads).
https://doi.org/10.1148/rycan.230155 © RSNA 2024
“It is important to share this knowledge with radiologists, thus allowing us to provide guidance to health care teams and assist with patient care,”
– Alok A. Bhatt, MD
Imaging Helps Identify Unexpected Complications, Early Recurrence
Head and neck cancer accounts for 3% to 5% of all malignancies in the U.S. with cancers originating from the lip, oral cavity, pharynx, larynx, nasal cavity and paranasal sinuses, salivary glands, and cutaneous soft tissues.
“Different treatment modalities can affect the head and neck in different ways,” Dr. Bhatt said. “Knowledge of the imaging findings seen after various treatment modalities can help distinguish post-treatment changes versus complications and recurrence.”
After treatment, patients may experience various expected changes, including mucositis, soft-tissue inflammation, laryngeal edema, and salivary gland inflammation, according to Dr. Bhatt. Imaging techniques such as CT, MRI and PET scans help differentiate these changes from tumor recurrence.
Dr. Bhatt and his team recommend a baseline contrast-enhanced neck CT and PET scan for patients 12 weeks after the completion of treatment for head & neck cancer.
“The goals of surveillance imaging are to distinguish expected findings from unexpected complications and early detection of recurrence,” Dr. Bhatt said.
Dr. Bhatt and his team also noted the treatment-related complications that can potentially occur, which include osteoradionecrosis, chondroradionecrosis, carotid blowout, fistula and discitis/osteomyelitis. Many of these complications can be identified early on in imaging and can be life threatening if left unattended. Chondroradionecrosis, for example can result in airway compromise.
“Imaging of head and neck cancer patients can make a true difference. We are often the first to recognize complications such as eminent carotid blowout or chondroradionecrosis,” Dr. Bhatt concluded. “This shows how valuable and integral of a role we can play on the multidisciplinary team.”
For More Information
Access the Radiology: Imaging Cancer article, “Imaging of the Posttreatment Head and Neck: Expected Findings and Potential Complications.”
Read previous RSNA News stories about cancer imaging: