Solving a Perplexing Puzzle: Radiology’s Role in the Diagnosis of Eating Disorders
Multisystemic manifestations can be seen at imaging


Eating disorders carry the highest mortality rate of any psychiatric disorder and affect 0.3% - 1.0% of the population. Despite their risks and prevalence, eating disorders often remain undiagnosed, in large part due to the associated social stigma.
It is important for radiologists to be aware of various imaging manifestations of eating disorders—many of which are nonspecific—to assist clinicians in reaching a diagnosis.
Nadia Solomon, MD, MSc, MA, and junior chief resident in radiology and biomedical imaging at Yale School of Medicine, New Haven, CT, said that if eating disorders are not considered as a possible cause of patient complaints, they can be easily overlooked or misattributed on imaging.
“The most common presentations of eating disorders are often nonspecific, such as chronic abdominal pain, chronic reflux, constipation or bloating,” Dr. Solomon said. “Moreover, patients do not tend to be forthcoming about their illness, which results in its being undiagnosed until the development of severe and even life-threatening complications. If you don't think to look for evidence of the diagnosis, you probably are not going to find it.”
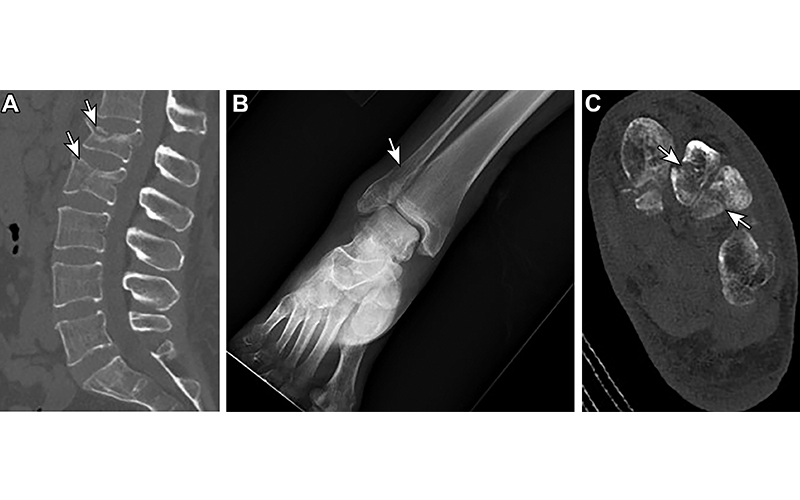
Osteoporosis and osteoporotic fractures in a 48-year-old woman with anorexia. (A) Sagittal nonenhanced CT image of the lumbar spine shows compression fractures of the L1 and L2 vertebral bodies (arrows). (B) Anteroposterior radiograph of the right ankle obtained on the same day as A shows a distal fibular fracture (arrow). (C) Axial nonenhanced CT image of the left foot confirms these fracture findings (arrows). https://doi.org/10.1148/rg.220018 © RSNA 2022
Imaging Findings Show Eating Disorders And Complications
Dr. Solomon, lead author of the RadioGraphics article, “Sequelae of Eating Disorders at Imaging,” emphasized that there are myriad, multisystemic imaging manifestations of eating disorders. Some radiographically apparent manifestations of restricting disorders include lack of body fat or low bone density, while purging disorders can manifest in esophageal laxity, gastritis and dental disease.
Lack of body fat may be noted on posteroanterior chest radiograph, indicated by a small heart shadow. Low bone density manifests on radiographs and CT with cortical thinning and hyperlucent bones and can lead to fragility or insufficiency fractures so subtle that they may only initially be seen on MRI. Laxity of the esophageal sphincter from repeated purging can lead to inflammation and subsequent thickening of the lower esophageal wall, a finding commonly seen in chronic reflux. While CT can demonstrate esophageal wall thickening, laxity of the lower esophageal sphincter is best demonstrated using fluoroscopy.
Margarita Revzin, MD, MS, associate professor of radiology and biomedical imaging at Yale School of Medicine and senior author of the article, also pointed out the importance of clinical history when identifying patients with eating disorders.
“Radiologists, particularly those in the Emergency Department, are like puzzle solvers who must connect the clinical information with the presenting radiological findings. Review of prior exams and how often a patient has presented with the same complaint can help establish patterns,” Dr. Revzin said. “There are many clues in a patient’s clinical history that can help radiologists solve the puzzle and make the diagnosis. Appreciation of one finding should inspire the radiologist to look for others.”
Emphasizing this point, Dr. Solomon noted, “An isolated finding may or may not be related to an eating disorder, because these tend to be multisystemic issues; however, if you notice one finding, and then start detecting other findings, it strengthens your suspicion that an eating disorder may be present.”
Other signs of eating disorders include health problems that are uncommon for a patient’s age, such as abnormally low bone mineral density in an adolescent or young adult patient, or an abnormally small or underdeveloped uterus in an adult patient who is expected to be hormonally mature.
Dr. Revzin encouraged radiologists to learn more about the imaging manifestations of eating disorders.
“Radiologists should be aware of this very common, but very complex spectrum of diseases and their effects on every system throughout the body,” Dr. Revzin concluded.
For More Information
Access the RadioGraphics article, “Sequelae of Eating Disorders at Imaging."
Read previous RSNA News articles on imaging for different body systems: