Preliminary Recommendations on Lymphadenopathy Associated with COVID-19 Vaccination
Emerging issue of particular concern to at-risk groups such as cancer patients






A routine follow-up PET scan of an oncologic patient left Daniel Steinberger, MD, assistant professor and a nuclear radiologist at the University of Minnesota, Minneapolis, puzzled.
The patient’s primary tumor had resolved, but there was new left axillary lymphadenopathy — which Dr. Steinberger was not expecting. To make matters even more puzzling, there was a triangle of intramuscular inflammation in the left arm musculature, something he had never seen before.
Dr. Steinberger initially interpreted the case as progressive disease, but the interpretation did not sit well with him.
Coincidentally, he was scheduled to receive his COVID-19 vaccine 15 minutes later. As he felt the poke from the needle in his arm, the explanation for the case became obvious. “The proverbial lightbulb went off and, going back and checking the patient’s record, I saw that the person had received a vaccination just days before the PET scan,” Dr. Steinberger said.
When he raised the issue at a departmental meeting, it became clear that his colleagues in breast, chest, body, head/neck and musculoskeletal imaging were all seeing similar cases. Digging a little deeper, they theorized that reactive axillary lymphadenopathy following COVID-19 vaccination could mimic metastasis in oncologic patients.
“We observed unilateral axillary lymphadenopathy in five patients using different imaging modalities, including PET/CT, MRI, mammography and ultrasonography,” Dr. Steinberger said. “While initial diagnosis was concerning for metastasis, further investigation revealed that these patients had all received their COVID-19 vaccination prior to imaging.”
A few days later, two patients elected to have biopsies and their theory was confirmed: The axillary lymph nodes were inflamed from the vaccine, not cancer.
A similar discussion was happening on the East Coast, at Memorial Sloan Kettering Cancer Center (MSK) in New York City.
“A number of our patients undergoing breast screening, as well as patients with treatment follow-up for lymphoma, melanoma and head and neck cancers, presented with unsuspected or sudden adenopathy,” said Hedvig Hricak, MD, PhD, chair of MSK’s Department of Radiology and a former RSNA president. “We realized that, in many cases, the adenopathy followed vaccination and it was always present on the side of the injection.”
Both sets of researchers published findings online in February in Radiology.
- The Case Series “Lymphadenopathy in COVID-19 Vaccine Recipients: Diagnostic Dilemma in Oncology Patients," by Dr. Steinberger and colleagues spotlights five cases of post-COVID-19 axillary lymphadenopathy that mimicked metastasis in oncologic patients.
- The Special Report, “Multidisciplinary Recommendations Regarding Post-Vaccine Adenopathy and Radiologic Imaging: Radiology Scientific Expert Panel," by Dr. Hricak and colleagues offers guidance from a panel of experts at three of the leading tertiary care cancer centers in the U.S.
“Hearing anecdotal reports of patients being biopsied for post-vaccination adenopathy, it became clear that we needed to raise awareness among both patients and physicians,” Dr. Hricak said. “This is obviously information that needs to be disseminated as widely as possible in order to prevent unnecessary investigations — including invasive biopsies.”
Know the Patient’s Vaccination History
Radiology researchers offer preliminary advice on dealing with COVID-19 vaccination-associated adenopathy.
“We collaborated with surgeons and medical oncologists, along with radiologists from various subspecialties, to come up with broadly applicable recommendations,” said Anton Becker, MD, PhD, a radiologist at MSKCC and lead author on the Radiology special report.
Included is a recommendation to question patients about their COVID-19 vaccination history.
“Ideally, a patient’s vaccination status will be clearly mentioned in all hospital documentation,” said Can Özütemiz, MD, a radiologist at the University of Minnesota and lead author on the Radiology Case Series. “However, because this is not always the case, imaging centers should prepare a pre-imaging questionnaire about recent COVID-19 vaccinations, particularly for those having mammograms, ultrasound, PET/CTs and CT of the neck and chest.”
“Communicating with patients and referring physicians is really the most important point, and this includes educating patients about the occurrence and significance of enlarged lymph nodes,” Dr. Becker said.
The authors of the Radiology Case Series also recommend watching for a triangle of intramuscular inflammation. “This could be indicative of vaccine-related inflammation and, if observed, should prompt one to inquire about the patient’s vaccination history,” Dr. Steinberger explained.
Recommendations Put Radiologists Ahead of the Curve
Considering the importance of getting vaccinated, especially for such at-risk groups as oncologic patients, both papers recommend postponing non-essential imaging for up to six weeks after a patient receives their final vaccination.
“If an imaging exam has been scheduled to take place shortly after a patient’s vaccination, but the exam can safely wait for six weeks, reschedule it to avoid the unnecessary anxiety provoked by findings of post-vaccination adenopathy,” Dr. Becker said.
“That said, we are also encouraging patients and clinicians to not delay clinically indicated imaging, such as acute clinical symptoms, already delayed screenings, short-interval treatment monitoring, or urgent treatment planning or complications due to prior COVID-19 vaccination,” added Sona Chikarmane, MD, a breast imaging specialist at Dana-Farber Cancer Institute and an author on the Radiology special report.
“When possible, patients should consider receiving the vaccine on the opposite side of a known or suspected cancer, such as in the case of breast, upper extremity melanoma or head and neck cancers,” added Melissa M. Chen, MD, a radiologist at MD Anderson Cancer Center, and an author on the special report.
Because there is no available data regarding the duration of radiologically evident lymphadenopathy or appropriate follow-up intervals, both papers recommend using the best available clinical judgement.
“Until such data becomes available, management must be guided by clinical context, particularly for those patients with a history of cancer with specific propensity towards axillary lymphadenopathy,” Dr. Özütemiz said.
Although neither of these reports are systematic, they effectively spotlight an issue that will become increasingly important in imaging and indicate a need for additional research.
“We have a unique opportunity to get ahead of the curve,” Dr. Hricak said. “By drawing attention to this issue early, we hope these initial studies help avoid unnecessary biopsies and follow-up examinations and the stress that such procedures place on our patients.”
Post-COVID-19 Vaccine Imaging Recommendations
Radiology experts offer recommendations for post-vaccine lymphadenopathy imaging, including:
- Perform imaging prior to the COVID-19 vaccine (when possible)
- COVID-19 vaccinations should not be delayed due to scheduled imaging for cancer patients and/or those undergoing cancer screening
- When required after the vaccine, do not delay imaging for urgent indications (acute symptoms, urgent treatment planning or complications)
- Consider postponing non-essential imaging for up to six weeks after a patient receives the final vaccination.
Educating Patients
Expert recommendations for educating patients about the expected side-effects of COVID-19 include:
- Every patient should take a pre-imaging questionnaire about recent COVID-19 vaccinations (date administered, injection site, laterality and type of vaccine)
- Radiologists should have immediate access to questionnaire responses
- Provide informational flyers in waiting rooms or with appointment letter using lay terms understandable on an 8th grade reading level
For More Information
Access the Radiology Case Series, "Lymphadenopathy in COVID-19 Vaccine Recipients: Diagnostic Dilemma in Oncology Patients."
Access the Radiology Special Report, "Multidisciplinary Recommendations Regarding Post-Vaccine Adenopathy and Radiologic Imaging: Radiology Scientific Expert Panel."
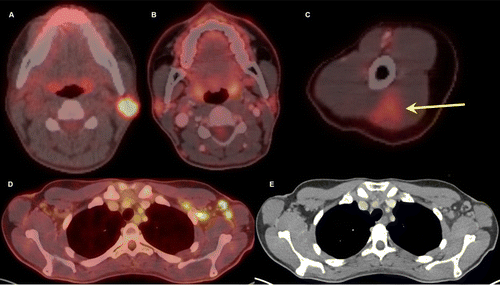
Thirty-two-year-old female. A, Axial fused 18-FDG PET/CT
showed hypermetabolic biopsy proven intraparotid lymph node with metastatic
malignant melanoma. B, Three-month follow-up axial fused 18-FDG PET/CT shows
complete resolution of the neck mass following chemotherapy, C, while left arm
shows hypermetabolic triangular shaped inflammation (arrow) at the COVID
vaccine injection site. D, Axial fused images at the axilla level shows
multiple new hypermetabolic lymph nodes. E, Axial contrast enhanced CT
demonstrates mild fat stranding surrounding the ovoid lymph nodes with
preserved fatty hilum.
Özütemiz et al, Radiology 2021 ©RSNA 2021