Platelet-Rich Plasma (PRP) has Potential for Injured Tendons, but Experts are Cautious
Athletes are embracing PRP but further investigation is necessary


Ultrasound-guided injections of platelet-rich plasma (PRP) into injured tendons represent the leading edge of a burgeoning field called orthobiologics that some musculoskeletal imaging experts believe has the potential to transform sports medicine.
Orthobiologics is the use of biological substances like PRP to help musculoskeletal injuries heal quicker. And while experts tout its potential, those same experts caution that the use of PRP is outpacing scientific evidence supporting it.
“No question, platelet-rich plasma has caught on,” said musculoskeletal radiologist Kenneth S. Lee, MD, professor of radiology and director of the Division of Musculoskeletal Imaging and Intervention at the University of Wisconsin School of Medicine and Public Health in Madison. “Unfortunately, the evidence isn’t quite there yet. More studies are needed.”
After PRP is drawn from venous blood spun in a centrifuge, it is injected into the affected tendon under US guidance. Its use in sports medicine began in 2006 and expanded rapidly as top athletes like Tiger Woods, Rafael Nadal and Stephen Curry embraced it as a way to treat injured tendons with minimal downtime. Media coverage and advertising amplified awareness of the procedure and soon even casual athletes were lining up for it.
“There has definitely been overutilization of orthobiologics,” Dr. Lee said. “There are many people out there trying to make money off it because insurance companies won’t pay for it, so they’re charging thousands of dollars for PRP or stem cells without much evidence.”
Watch Dr. Lee talk about the use of PRP for injured tendons:
Dr. Lee has seen interest in PRP firsthand from athletes in the University of Wisconsin’s high-powered collegiate sports programs. Much of the interest, he said, is driven by the large number of people with sports-related repetitive motion injuries who fail to benefit from conservative therapy but aren’t candidates for surgery.
“There’s this gap in treatment between those who have mild or minor disease and get better with rest and those who need surgery,” said Dr. Lee, who presented in an RSNA 2020 Controversy session on PRP and musculoskeletal injectables. “The people in between those two groups who suffer from chronic tendon injuries are often desperate and willing to try anything.”
In theory, PRP works by introducing platelets and growth factors that are secreted after platelet activation into the injured tendons, triggering a healing response that helps reverse structural damage. In practice, results have been mixed.
Dry Needling is Effective Alternative
A 2010 study in the American Journal of Sports Medicine on people with tennis elbow concluded that PRP was much better than steroids in terms of improvements in function and reduction in pain over time.
However, another study published that same year in the Journal of the American Medical Association found that PRP was no better than a saline injection in treating Achilles tendinosis.
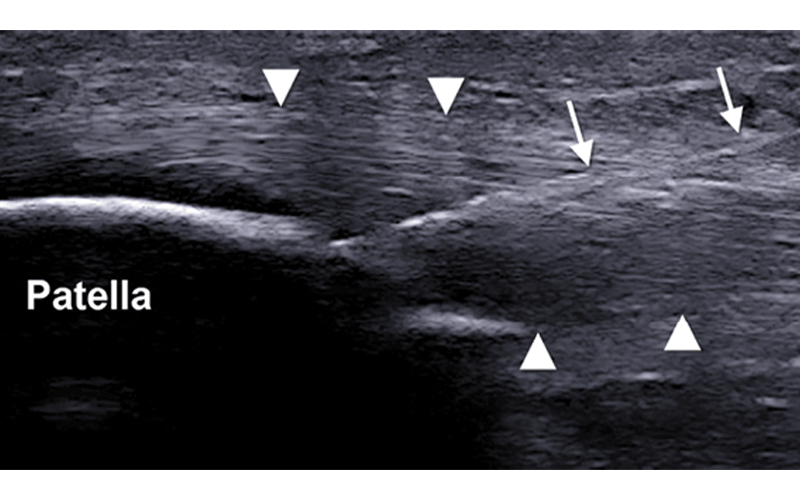
Results from a 2014 study in the American Journal of Sports Medicine on patellar tendinosis showed that, in the short term, PRP was better than dry needling, a technique in which a needle is introduced into the damaged area of the tendon to trigger a healing response. That advantage was lost at about 26 weeks post-treatment.
“Most papers have found no difference in outcomes between PRP and dry needling,” said Jon Jacobson, MD, professor of radiology and director of the Division of Musculoskeletal Radiology at the University of Michigan in Ann Arbor. “They both work and approximately 70% to 80% of patients show improvement regardless of which treatment they receive.”
Similar outcomes have also been found for whole blood injections, in which blood is removed from the patient and injected into the site of the injured tendon without any additional preparation. The similarities may be related to the fact that needling is part of the process of injecting PRP, whole blood or any other orthobiologic.
“If I’m injecting PRP, I’m going to fenestrate the tendon to make space for the PRP,” said Dr. Jacobson, who has published multiple studies on dry needling for chronic tendinosis. “One theory of why PRP and dry needling have similar outcomes is that the underlying process of needling the tendon is present with both procedures.”
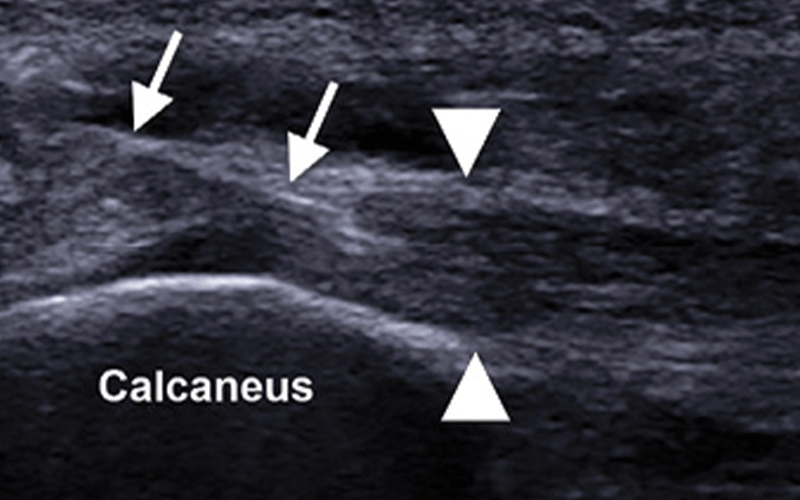
Some of the strongest evidence favoring PRP came from a study Dr. Lee conducted on subjects with plantar fasciitis.
The study, “Acoustoelastography as an Outcome Measure for Platelet-Rich Plasma Injection Treatment of Chronic Plantar Fasciitis: A Pilot Study,” was funded by a 2010–2011 Toshiba America Medical Systems/RSNA Research Seed Grant.
In the study, half of the 44 subjects received PRP while the other half received steroids. Both groups experienced improvements in pain and function, but the PRP group continued to improve at the 32-week mark, just as the steroid group reported increased pain levels.
“Since we began researching PRP at the University Wisconsin 10 years ago, I’m more comfortable in saying that it is effective for treating tendinosis,” Dr. Lee said.
Costs Vary Widely
PRP faces a number of hurdles, starting with cost. Because it is still considered an experimental procedure, PRP is rarely covered by insurance and out-of-pocket cost to the patient starts at about $500.
Dry needling, in contrast, is covered by most insurance companies as a tendon injection and patients are typically only responsible for a small copay of $20 to $30.
Dr. Jacobson says that patients often request PRP because they’ve heard about famous athletes undergoing the procedure. While he ultimately leaves the final call up to the patient, he discusses the scientific evidence with them before they make their decision.
“I tell patients with tendinosis that I will offer them dry needling, whole blood injection or PRP, and then I explain to them that the literature shows no difference in outcomes among the three,” Dr. Jacobson said. “The big difference is cost.”
Injectable stem cells are harvested from the patient’s own fat or bone marrow before they are injected into the tendon. As with PRP, the idea is that stem cells will encourage healing of the damaged tendons.
Dr. Lee isn’t so optimistic. A recent literature review found no evidence that stem cells are effective for treating chronic tendon injuries.
“The reality is, we don’t carry that many stem cells and as we age the level drops precipitously, so the whole premise doesn’t make a lot of sense,” he said.
Until more research becomes available, musculoskeletal imaging experts like Drs. Lee and Jacobson will remain wary of endorsing PRP over the far less expensive dry needling approach.
“I’m not going to ask for $600 from a patient if I know in my heart that the outcome may not be be any better than what they would get from dry needling for a $20 copay,” Dr. Jacobson said.
For More Information
Access Dr. Lee’s related research at the University of Wisconsin at Radiology.wisc.edu/research.
Connect with Dr. Lee on social media @kenlee8799 or @UW_MSKrad
Connect with Dr. Jacobson on social media @jjacobsn
Read previous RSNA News stories on musculoskeletal radiology: