Weight Loss Surgery Improves Breathing Issues in Obese Patients
Obesity can harm the respiratory system leading to additional impairments

Bariatric surgery and weight loss appear to reverse some of the negative effects of obesity on the respiratory system, according to a study published in Radiology.
Known effects of obesity on the respiratory system include increased respiratory work, along with compromised airway resistance and respiratory muscle strength, which may all contribute to restrictive pulmonary function impairment.
CT has great potential to improve understanding of obesity’s impact on the respiratory system. Up until now, however, there have been few CT studies evaluating obesity’s effects on the lungs and the trachea.
Study lead author Susan J. Copley, MD, observed differences on chest CT images obtained in obese patients in her practice as a thoracic radiologist at Hammersmith Hospital in London, part of Imperial College Healthcare NHS Trust.
“This caused me to wonder if these differences were due to obesity and whether they were reversible after weight loss,” she said.
CT Can Document Improvements in Respiratory Efforts Following Weight Loss
Dr. Copley and colleagues evaluated changes in the respiratory systems of 51 obese individuals who underwent bariatric surgery. All participants lost weight post-surgery with a mean body mass index decrease of 10.5 kg/m2.
The researchers used CT to measure the size and shape of the trachea and assess air trapping, resulting in a reduction in lung function.
When the researchers compared results at baseline and six months after bariatric surgery, they found that surgery and weight loss were associated with morphological changes to the lung and trachea.
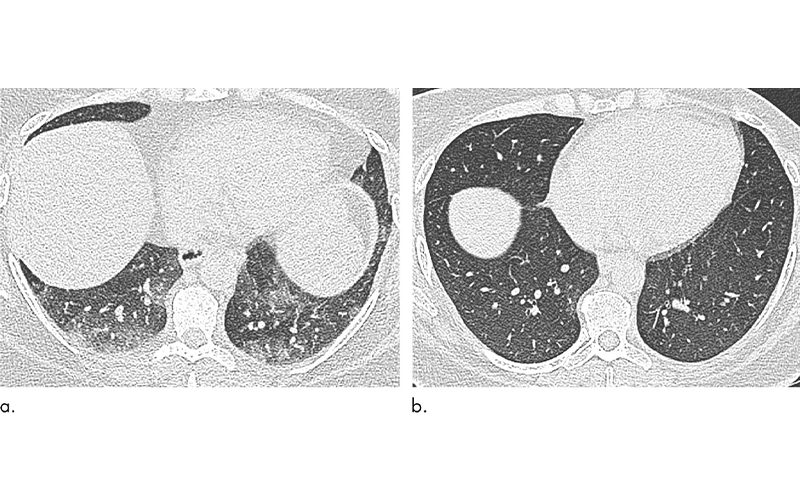
Post-surgery CT showed reductions in air trapping and a lower incidence of tracheal collapse. Change in the extent of CT air trapping was the strongest predictor of improvement in dyspnea.
“For the first time, this study has demonstrated changes in the CT morphology of large and small airways that improve when individuals lose weight,” Dr. Copley said. “These features correlate with an improvement in patient symptoms.”
The results suggest that there may be a reversible element of small airway inflammation related to obesity and that reversal of this inflammation correlates with improvement in symptoms. The findings also point to CT as a potential marker of this inflammation.
While more studies are needed to better understand the link between CT features and biomarkers of inflammation, the study underscores CT’s potential in the work-up of patients with obesity.
“CT is a useful morphological marker to demonstrate subtle changes which are not easily assessed by lung function alone,” Dr. Copley said.
For More Information
Access the Radiology study, “Lung Parenchymal and Tracheal CT Morphology: Evaluation Before and After Bariatric Surgery."