Intensive Blood Pressure Lowering Safe, Beneficial for Brain Health
Review over time showed improvement in connectivity of key brain areas


According to the World Health Organization, an estimated 1.28 billion adults aged 30 to 79 have hypertension. Considered a risk factor for heart disease, stroke and chronic kidney disease, it can also have significant impact on the brain, including causing cognitive dysfunction.
In a study funded in part by a 2019 RSNA Research Fellow Grant, Chintan Shah, MD, now a staff neuroradiologist and informaticist at Cleveland Clinic, worked with fellow researchers at the University of Pennsylvania in Philadelphia using MRI and fMRI to assess the impact of standard and intensive blood pressure management in helping preserve brain functional connectivity in adults with hypertension.
The Systolic blood Pressure INTervention (SPRINT) trial, initiated in 2010 and funded by the National Institutes of Health, was designed to evaluate the effect of treatment targeting systolic blood pressure with a goal of lowering it from the prior target of 140 mmHg to 120 mmHg.
“The original SPRINT trial demonstrated that intensive management of high blood pressure improved cardiovascular outcomes compared to standard treatment and served as one key piece of evidence for redefining what we now classify as hypertension,” Dr. Shah said.
He noted, however, that within the SPRINT trial, the intensive therapy group saw a slight increase in adverse effects, such as syncope and hypotension, that raised the question of whether this approach was safe and effective for brain health.
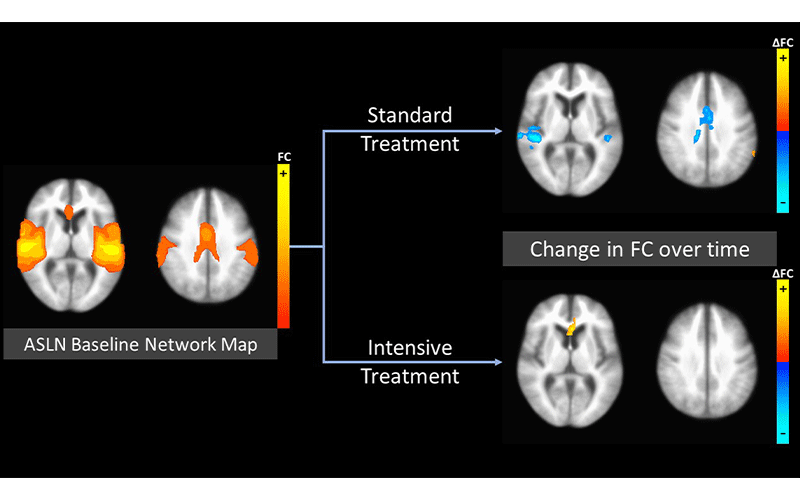
Caption: Baseline network map and change over time for the auditory-salience-language network (ASLN). Left image shows a group average functional connectivity (FC) network map for the ASLN at baseline. Right images show areas of change over time in the network. In the Standard Treatment group, there are areas of negative longitudinal change in the temporal lobes (right more than left), right posterior insula, and anterior cingulate region. These areas do not show substantial change in the Intensive Treatment group. Photo provided courtesy of Chintan Shah, MD.
Study Evaluates Longitudinal Changes in Brain Network Connectivity
The initial SPRINT trial randomized 9,361 adult subjects aged 50 or older with hypertension to receive either standard blood pressure treatment, targeting systolic blood pressure at <140 mmHg or intensive blood pressure treatment targeting systolic blood pressure at <120 mmHg.
To begin examining the impact of the intensive treatment on brain function, Dr. Shah and his team first conducted a study that was later published in Neuroradiology. It included a subset of 550 trial participants who underwent brain MRI, including resting state functional brain MRI, to evaluate the strength of different brain networks.
“We first assessed the cohort at baseline prior to randomization to determine how structural changes such as white matter hyperintensities (WMH) were related to the functional connectivity of brain networks,” Dr. Shah said.
He and his colleagues noted that a greater burden of WMH is related to decreased functional connectivity of several brain networks, including that of the default mode network, which was then related as a mediating factor to cognitive test performance.
At RSNA 2021, the researchers presented results of a follow-up longitudinal study, in the setting of the SPRINT randomized control trial, comparing the change over time in the connectivity of specific brain networks between the two treatment groups.
“In this study, intensive therapy was associated with a small improvement over time in connectivity of the auditory-salience-language network, compared to standard therapy which showed a small decrease over time,” Dr. Shah said.
He said that connectivity changes were most prominent in the brain areas corresponding to the salience network, the regions of the brain that detect behaviorally relevant stimuli and for coordinating the responses to these.
“These areas showed less decline in the intensive treatment group, however the changes were not related to change in overall brain volume or total volume of white matter hyperintensities,” Dr. Shah said. “This suggests that additional mechanisms may be involved in cognitive dysfunction in hypertension.”
The results of the study validate the safety and benefit of intensive blood pressure lowering for both cardiovascular and brain health.
“Our results serve to promote adoption of the most recent American College of Cardiology and American Heart Association guidelines for treatment of hypertension earlier and with a lower target blood pressure, compared to prior guidelines,” Dr. Shah said.
R&E Funding Provided Access to Time, Resources
Dr. Shah noted that the R&E Foundation grant was instrumental in allowing him to complete his research by providing him with sufficient time, resources for support staff and analysis, and helping aid his unexpected transition to remote work during the COVID-19 pandemic.
“Both work and personal schedules were altered and in flux, and in particular, child care became more challenging,” he said.
A one-year, no cost extension of the grant helped him continue the research primarily on a remote basis. As a second-year fellow with busy clinical duties, he was challenged to complete the full study image processing on his own and noted that the grant assisted with funding for an image analyst to help with the large volume of studies. He was also able to invest in a computational workstation.
“There were many challenges that came along with balancing the demands of this research project, including its setbacks, alongside other projects, clinical duties, training requirements and personal responsibilities,” Dr. Shah said. “I believe that receiving this grant and having dedicated time at an earlier point in my career has helped me develop skills in balancing and prioritizing these responsibilities.”
For More Information
Learn more about R&E Foundation grants at RSNA.org/Research/Funding-Opportunities.
Read previous RSNA News stories about R&E Foundation grants: