Groundbreaking Postoperative Hip Dislocation Risk Calculator
Machine learning and imaging combine to create patient-specific risk and surgical planning tool



After the first FDA-approved total hip arthroplasty (THA) was performed at Mayo Clinic in 1969, the clinic began a total joint arthroplasty registry to follow all patients’ outcomes throughout their lifetimes.
Now, in a study in Radiology: Artificial Intelligence, data from this registry has been combined with imaging and machine learning to produce a risk calculator capable of predicting patient risk of postoperative hip dislocation within five years.
Deep Learning Assists with Surgical Planning
Hip implant dislocation is the most common complication of THA, occurring in among 4%-5% of patients. It is treated by reduction under sedation and in cases of chronic dislocations, revision surgery.
THA is the second most common elective surgery in the U.S., and is expected to triple in incidence by 2040 as the population ages.
Orthopedic surgeons can mitigate dislocation risk through certain surgical variables, but predicting which patients are at risk currently relies on the evaluation of patient comorbidities. With the use of the risk calculator, it is hoped that surgeons can make more informed surgical decisions.
“There are some decisions that the surgeon can make to change the patient’s risk of dislocation, such as how they perform surgery or what type of implants they use,” said Bardia Khosravi, MD, MPH, MHPE, radiology post-doc fellow at Mayo Clinic in Rochester, MN. “What we wanted to do was give surgeons a tool to see how different combinations of those decisions will affect the patient’s risk of dislocation.”
“There are some decisions that the surgeon can make to change the patient’s risk of dislocation, such as how they perform surgery or what type of implants they use. What we wanted to do was give surgeons a tool to see how different combinations of those decisions will affect the patient’s risk of dislocation."
– BARDIA KHOSRAVI, MD, MPH, MHPE
Using Data to Train the Algorithm
The deep learning calculator improves on an existing calculator that factors in clinical data only. Using a machine learning–based pipeline allows researchers to evaluate the risk of dislocation based on a single preoperative anteroposterior (AP) radiograph, as well as clinical characteristics.
“We have a large database of images and their clinical outcomes, so we know whether or not patients dislocated after surgery,” explained co-author Bradley J. Erickson, MD, PhD, and professor of radiology at Mayo Clinic. “We trained the deep learning algorithm to figure out which configuration of imaging features and patient comorbidities is likely to lead to dislocation.”
This retrospective study included 17,073 patients who underwent primary THA between 1998 and 2018. Patient charts were reviewed to extract demographics, relevant comorbidities and surgical characteristics. A representative set of 10% of these patients was randomly selected to be used as a holdout test set.
Using each patient’s latest preoperative AP radiograph and clinical characteristics, a series of machine learning algorithms focused on image classification, feature extraction and survival analysis was designed to predict dislocation risk. The researchers developed two prediction models: one using clinical information only and the second using clinical information in combination with imaging data.
A graphical user interface on the calculator was also developed to facilitate clinical use and ensure explainability of the model.
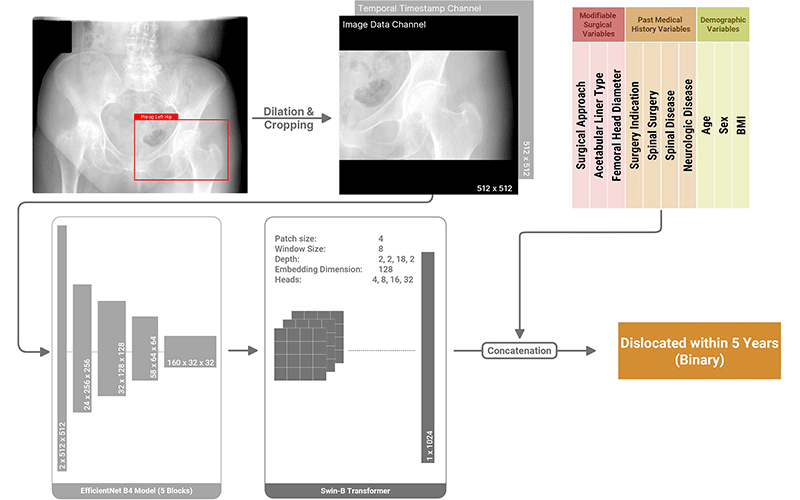
Proposed architecture for the deep learning multimodal classifier.
https://doi.org/10.1148/ryai.220067 ©RSNA 2022
Robust Predictions Powered by Imaging
“The model hat added a preoperative radiograph to the mix correctly predicted dislocation risk 74% of the time, compared to 64% for the model that used clinical information only,” Dr. Khosravi said.
Co-author Cody C. Wyles, MD, assistant professor of orthopedic Surgery and clinical anatomy at Mayo Clinic, affirmed from an orthopedic perspective that the multimodal model’s predictions are powered by imaging.
“The preoperative image, knowing nothing else about these patients, was the most predictive metric,” Dr. Wyles said.
“In orthopedic circles, we think we know what the clinical and surgical variables are that matter. Yet this deep learning model, just looking at an X-ray before surgery even happened, had a better ability to predict which patients would dislocate.”
Potential to Adopt Model in Health Care Settings
Fortunately, the data needed by the calculator is already part of the patient workup to THA, including preoperative AP radiographs and the gathering of standard clinical information.
“The AP radiograph is a very standard procedure, and almost always done prior to hip arthroplasty,” Dr. Erickson said.
Dr. Wyles noted that the risk factors listed on the calculator’s user interface are typical questions the surgeon asks in the patient workup.
“We looked at a lot of different potential variables, and the deep learning algorithms boiled them down to just a handful that were the most predictive,” Dr. Wyles said. “Serendipitously, these variables are questions that we already ask our patients at their first appointment.”
In addition, the multimodal model learned from images acquired from over 100 different X-ray machines, making it adaptable enough to analyze images in almost any health care setting.
“The data covers many different types of radiographs,” Dr. Khosravi explained. “We trained the model so that it doesn’t rely on a specific type of scanner.”
To see how well the calculator performs in real time, Mayo Clinic has begun a prospective study.
“We’re prospectively studying this calculator to see how it improves outcomes over time,” Dr. Wyles said. “We’ve launched it internally here at Mayo Clinic, and once we get more feedback from users, we hope to have it more broadly available.”
FOR MORE INFORMATION
Access the Radiology: Artificial Intelligence study, “Patient-specific Hip Arthroplasty Dislocation Risk Calculator: An Explainable Multimodal Machine Learning–based Approach.”
Read previous RSNA News stories about machine learning: