Persistent Pulmonary Manifestations in Children Following COVID-19
Low-field MRI demonstrates changes in lung parenchyma for children and teens with long-COVID



Children and teens who have had COVID-19 tended to have milder disease compared to adults with recovery within a few weeks. While there is increased understanding of the multi-organ damage of COVID-19 beyond the acute phase of infection, the nature, frequency and definition of post-acute infection in children and teens remains unknown.
CT has aided in the diagnosis of pulmonary changes due to COVID-19 in adults, showing changes in pulmonary microcirculation in up to 65% of patients. However, studies using ionizing radiation are not feasible in children, and the lung parenchymal changes due to COVID-19 that are seen in children are less obvious or pronounced on CT.
In a Radiology study, Rafael Heiss, MD, from the Institute of Radiology, and Ferdinand Knieling, MD, from the Translations Experimental and Molecular Imaging Laboratory in the Department of Pediatrics and Adolescent Medicine, both at the University Hospital Erlangen, Friedrich-Alexander-Universität (FAU) Erlangen-Nürnberg, Germany, and colleagues, utilized low-field MRI to determine the morphologic and functional changes of lung parenchyma in children and adolescents with post COVID-19 compared to healthy controls.
“The main function of the lungs is to bring oxygen-depleted blood into contact with the inhaled air. For this purpose, both functions must overlap. We showed that this is true for about 90% of the lung tissue in healthy children,” Dr. Heiss said. “For children who had had a previous COVID infection, we found that previous infection leads to a decrease in this ‘normal’ function of the lungs, regardless of whether the children had persistent symptoms or not. This means, on the one hand, that an infection still produces persistent dysfunction even after months and, on the other hand, that not all children will be clinically affected in the same way.”
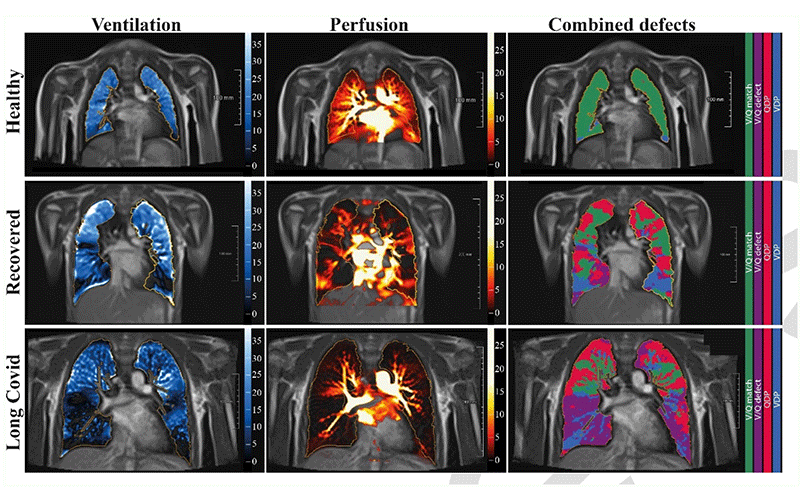
Free-breathing phase-resolved functional lung (PREFUL) low-field MRI at 0.55T with calculated parameters at an axial plane after automatic registration to a mid-expiration position and lung parenchyma segmentation. From left to right, representative color-coded images of functional show ventilation defects (VDP, blue), perfusion defects (QDP, red), ventilation/perfusion (V/Q match, green), ventilation/perfusion defects (V/Q defect, purple) in a healthy control (upper row, 7-year-old male), a participant recovered from COVID-19 (middle row, 10-year-old male) and a participant with long COVID (15-year-old male).
https://doi.org/10.1148/radiol.221250 ©RSNA 2022
Children With Long COVID Showed Functional Changes of Lungs With Low-Field MRI
For the study, a cross-sectional, prospective clinical trial using low-field MRI was performed in 54 children and adolescents with previous SARS-CoV-2 infection (29 recovered, 25 with long COVID) and results were compared with nine healthy controls from a single academic medical center.
The definition for long COVID reflects the current WHO definition and is based on the persistence of symptoms for a minimum of 12 weeks. It also includes symptoms that persisted from the acute COVID-19 phase or its treatment or that resulted in a new health limitation, new symptoms that occurred after the end of the acute phase but were understood to be a consequence of COVID-19 disease, or the worsening of a pre-existing underlying medical condition.
Of the 25 participants classified as having long COVID, 16 reported shortness of breath (30%), five reported headache (9%), 15 reported dyspnea (28%), six reported impaired attention (11%), four reported anosmia (7%), and four reported fatigue (7%). Pneumonia, loss of taste and limb pain were each reported by one participant (2%).
Eligible patients were required to have a documented positive RT-PCR-test for SARS-CoV-2. Healthy controls were excluded when previous positive SARSCoV-2 infection confirmed by RT-PCR or rapid antigen test and any clinical or other suspicion of pulmonary disease, respiratory infection/symptomatology or pain resulting in respiratory limitation.
All participants underwent morphological and functional low-field MRI to visualize morphological features, ventilation and perfusion of the lungs. Ventilation/perfusion (V/Q) matches were 81 ± 6% in healthy controls, 62 ± 19% in the recovered group, and 60 ± 20% in the long COVID group. V/Q matches were lower in post COVID participants with infection less than 180 days (63 ± 20%), 180 to 360 days (63 ± 18%) and 360 days (41 ± 12%) compared to never-infected healthy controls (81 ± 6.1%).
“We observed a more pronounced decrease in functional lung parenchyma depending on how long ago the infection occurred,” Dr. Knieling said. “This means that children and adolescents who were infected at the beginning of the pandemic had more pronounced changes on average. It remains unclear whether this is related to the predominant viral variant, the small corhort or other study related effects.”
More Research Needed to Understand COVID-19 Effects in Children
This study expands the understanding of pediatric post-acute COVID-19 disease, particularly given the increased incidence of SARSCoV-2 infection. A better estimate on the prevalence of pediatric post COVID lung disease is further complicated by the inconsistent, largely symptom-based definitions of long COVID disease and its limited applicability to children.
“One reason that long COVID is difficult to identify in children and teens is that there is no international consensus regarding the definition of long COVID in children or agreement on the duration of symptoms required to make this diagnosis,” said Harriet J. Paltiel, MD, a pediatric radiologist and associate professor of radiology at Boston Children's Hospital and Harvard Medical School, associate editor of Radiology and author of an accompanying Radiology editorial. “Although a large number of symptoms have been attributed to pediatric long COVID, many are nonspecific and very common in the general population. In addition, the nature and frequency of the sequelae of acute COVID infection in children are poorly understood since there have been no long-term follow-up studies reporting patient outcomes. Most of the studies that have been published have used questionnaires where the patients or their parent’s reported symptoms but did not include clinical assessment or objective documentation such as imaging findings or pulmonary function testing.”
Dr. Heiss concurred.
“Pediatric patients, who often have no preexisting conditions, can compensate for functional changes for much longer. A reduction in physical performance, as was obviously seen in our long COVID group, can thus easily be overlooked even in ‘asymptomatic’ patients. Functional measurements, as shown by our study, could help to obtain more objective findings without exposing patients to additional radiation.”
The further course and outcome of the observed changes remains unclear.
“The research investigation in this study provides objective documentation of ventilation-perfusion mismatches in symptomatic patients at a particular point in time, but the clinical significance of these abnormalities is, as yet, uncertain,” Dr. Paltiel said. “It will be necessary to correlate the MRI findings with pulmonary functional and vascular abnormalities documented with conventional ventilation-perfusion scintigraphy, hyperpolarized 129Xe MRI, and/or standardized pulmonary function testing. Longitudinal patient evaluation with repeat low-field strength MRI should also reveal whether or not the previously documented abnormalities are transitory or permanent, and how they compare to serial pulmonary function evaluation and clinical symptomatology.”
Dr. Knieling noted that the next step is to initiate a follow-up trial.
“We would want to look at the changes over a longer time frame and try to correlate them to other organ findings, such as capillary microcirculation,” Dr. Knieling said. “We want to find out whether our results are only a snapshot, due to the prevailing virus variant.”
For More Information
Access the Radiology study, “Pulmonary Dysfunction after Pediatric COVID-19 and the accompanying editorial, “Low-field MRI and ventilation-perfusion mismatch after pediatric COVID-19."
Read previous RSNA News stories on pediatric COVID-19: