Creativity, Collaboration Help Radiology Departments Choose Appropriate Sedation for Children
Strategies help children avoid sedation while reducing anxiety to ensure high quality imaging



With a combination of consistent triaging, flexible scheduling, multidisciplinary cooperation and supportive technology, radiology departments can confidently reduce anesthesia use in children undergoing imaging procedures.
“Processes need to be standardized and streamlined as much as possible to make it easy to reliably do the right thing,” said Evan J. Zucker, MD, clinical associate professor at Stanford University School of Medicine and Stanford Children’s Health in Palo Alto, CA.
Keeping children motionless for imaging procedures, particularly for lengthy MR exams, can be a tricky business, and often the simplest choice for medical staff is general anesthesia. But there are more options for squirmy kids, successful program leaders say. In the November-December 2021 issue of RadioGraphics, Dr. Zucker and colleagues published their findings on how a radiology department can implement—and successfully execute—a program that utilizes “moderate sedation” in place of deep sedation or anesthesia when appropriate.
Such a program had been in place for some time at Stanford, but it was seldom adhered to, despite many children meeting eligibility. Through a five-month quality improvement initiative, Dr. Zucker’s multidisciplinary team identified what was driving low utilization and, subsequently, launched a plan to fold moderate sedation more seamlessly into the workflow.
“Our Pareto analysis demonstrated that the most common reason exams were not being scheduled with sedation was the lack of completion of the sedation screening checklist by the protocolling nurse,” Dr. Zucker explained. “There were several factors likely contributing to this, including a large, heterogeneous group of nurses with variable training and experience, and the requirement that the checklist had to be manually inserted into the chart and could be forgotten. Additionally, the multiple questions on the checklist required a deep dive into the medical record.”
The alternative option, Dr. Zucker said, was simply selecting general anesthesia—which was less complicated and time-consuming. Nurses often went with the simpler choice.
Anesthesiologist Buy-In Enables a Backup Plan
To address these impediments, the Stanford team tried a multifaceted approach to screening and scheduling.
They consulted with sedation hospitalists and the RN manager to establish clearer definitions of eligibility for moderate sedation, provide coaching and standardize the protocol workflow for technologists and nurses. Automated changes to electronic record entry set the course. For example, previously the question, “Does this patient need general anesthesia?” could only be answered with “yes,” “no,” or “unsure.”
The automatic process only routed the “unsure” records through moderate sedation. In the updated version, a new question—“Does this patient need some level of anesthesia to remain still during the examination?”—allowed both “yes” and “unsure” records to be considered.
At the program’s peak, the department achieved as much as 88.9% success for exams completed with moderate sedation and even after the pilot period ended— amidst the initial COVID-19 wave—success rates remained similar.
Dr. Zucker’s team also established a formal plan for children whose exams couldn’t be completed with moderate sedation, keeping anesthesiologists on hand for a same-day salvage with general anesthesia whenever resources were available. Although this potentially meant more work, the team agreed that the approach aligned with patient service and satisfaction. And, as it turned out, moderate sedation attempts rarely failed.
Technology, Technologists Steady the Course—and the Kids
At the Boston Children’s hospital, Sarah Bixby, MD, MBA, the Paul Kleinman chair of MSK imaging and medical director of MR imaging said a “Try Without Anesthesia” program has been in place for more than 10 years. Her department’s approach is to double-book appointments. They schedule a “Try Without” appointment plus a general anesthesia appointment several weeks in the future.
“If we get the exam done during the Try Without appointment and the images are of diagnostic quality, then we just cancel the anesthesia appointment,” Dr. Bixby said.
The Boston Children’s program employs a toolset of creative child guidance and top-notch technology. They’re equipped with fast-sequence scanners to reduce imaging time, but they also provide engagement to curb the wiggles during a scan.
“We have sound systems and video goggles that the children can wear right in the scanner, and they can watch movies or participate in motion-reduction activities,” Dr. Bixby said. “There’s also the option to practice on a simulation unit. The simulator makes the same sounds as a real coil and children can see what it’s like inside the bore and even run a doll or a stuffed animal through the exam process.”
When it comes to staff-and-child interactions, the best team is one who knows their young patients, according to Dr. Bixby.
“We have a child life specialist on staff, and we also have an amazing team of technologists who are great with kids,” she said. Parents of infants and toddlers are encouraged to book exams that coincide with their children’s sleep schedules— appointments are available as late as 9 p.m.—to increase the likelihood that the child will simply nap through the imaging.
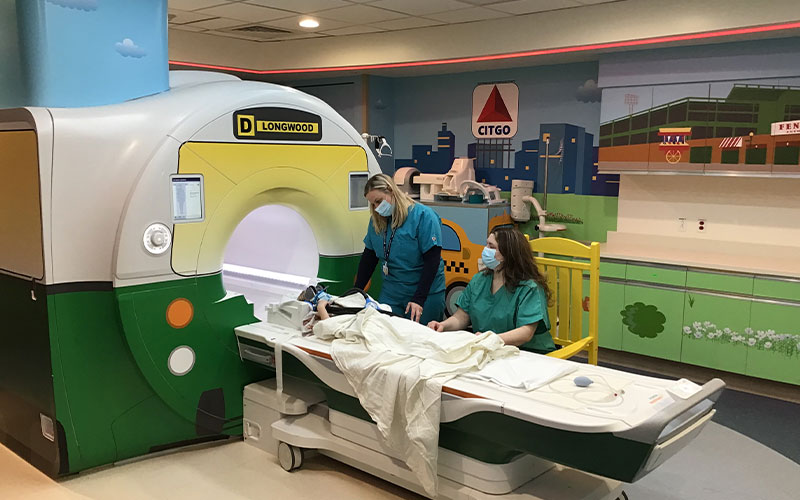
At Boston Children's Hospital, the MRI suite and scanner are outfitted to resemble a subway car.
Hong Kong Experience Embraces Collaboration, Inspiration
Mock scanners and bedtime scheduling are also big at Hong Kong Children’s Hospital (HKCH), where radiology and anesthesiology staff have adopted an approach that’s cooperative by default.
“At HKCH, an anesthesia-led sedation team is responsible for the majority of sedation services for children undergoing radiological procedures,” said Elaine Kan, FHKCR, chief of service of the Department of Radiology.
With the exception of complex, high-risk, or potentially painful procedures, HKCH’s default is sedation rather than general anesthesia, Dr. Kan explained.
“For those whom sedation is not indicated, anesthesiologists may refer patients to the radiology team for feed-and-sleep, mock scans or non-sedation as appropriate,” she said.
“Feed-and-Sleep” is a collaborative program with HKCH’s Department of Anesthesiology and Perioperative Medicine.
“With careful selection of patients by the anesthesiologist, we make use of patients’ daily feed and natural sleep pattern to let babies and young children fall asleep before we start scanning,” Dr. Kan explained.
For children who’d rather be enchanted than asleep, the child-centered imaging facilities at HKCH provide a uniquely fun experience.
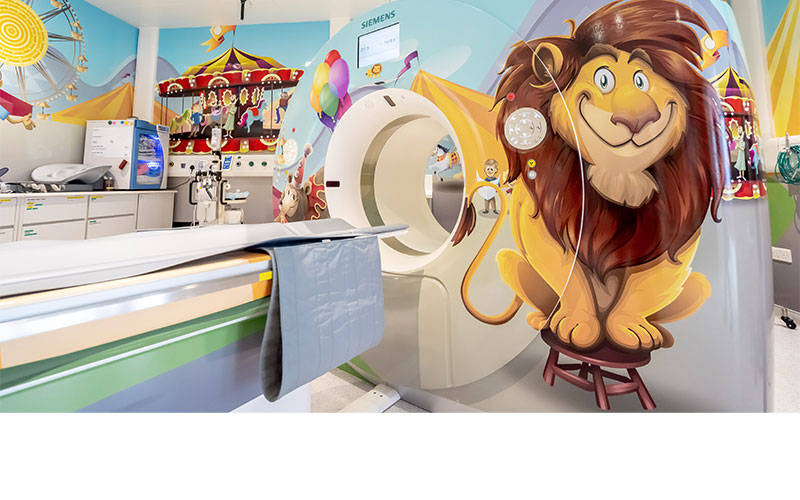
“Our team of radiologists, radiographers and nurses gathered up our creativity and converted the original plain, white and cold department into a theme park,” Dr. Kan said. “The general X-ray room is decorated like a spaceship, the ultrasound room is a ‘night safari’ covered with glow-in-the-dark stars, the CT scan room has a circus theme and the MR scan room is decorated as an ocean. Many of our patients enjoyed their experiences so much that they requested to stay in the department when their examinations were completed!”
Choosing the right path for sedation in children remains daunting and challenging, Dr. Zucker said.
“Rather than get consumed by the enormity and complexity of pediatric sedation, break down the problem into smaller pieces, establish baseline metrics and commit yourself to a measurable goal and timeline,” Dr. Zucker advised. “Most importantly, understand the institutional culture, and involve key stakeholders— nurses, technologists, child life specialists and anesthesiologists. Test small interventions and celebrate successes, but don’t be afraid to fail.”
In the longer term, radiology teams should think about making processes simple and reliable, such as through the effective use of IT tools, Dr. Zucker continued.
“Improvement and change are seldom easy, but the end result is providing better care to patients, and we can all agree that is our ultimate purpose,” Dr. Zucker concluded.
For More Information
Access the RadioGraphics article, “Increasing the Utilization of Moderate Sedation Services for Pediatric Imaging."
Read previous RSNA News stories on pediatric radiology:
RadiologyInfo.org Offers Variety of Patient-Friendly Pediatric Imaging Resources
Radiologists can help parents and caregivers with children scheduled for imaging by directing them to RadiologyInfo.org.
The public information website produced by RSNA and ACR offers easy-to-understand information, videos and pictures of more than 250 procedures, exams and disease topics. This information is offered in English and Spanish.
The RadInfo4Kids section offers videos, stories and games geared toward children who have an upcoming imaging exam. The pages explain imaging tests and treatments in a way that children can understand to help ease any fears about their exam.
Visit RadiologyInfo.org for all of these resources.