Including Radiation Dose Distribution Maps in Medical Records May Enhance Cancer Care
Readily available radiation dose history an increase the ease and accuracy of image interpretation

When a patient undergoes radiation therapy for cancer, radiation oncologists create a radiation dose distribution map — a visual representation of the dose given to each anatomic structure volumetrically.
While a radiation dose distribution map is a critical part of a patient’s medical record, it is not easily accessible to all of a patient’s medical providers — but it should be, according to Ricky R. Savjani, MD, PhD, resident physician in the Department of Radiation Oncology at the University of California Los Angeles (UCLA).
Dr. Savjani is the lead author of, “A Framework for Sharing Radiation Dose Distribution Maps in the Electronic Medical Record for Improving Multidisciplinary Patient Management,” recently published in Radiology: Imaging Cancer.
“Having ready access to radiation dose maps can directly improve patient care across many health care settings,” Dr. Savjani said. “In the emergency department, for example, knowing precisely when and where a patient has had previous spine radiation can help a physician triage the person with spinal cord compression to determine the most appropriate treatment more rapidly.”
Watch Dr. Savjani discuss including radiation dose distribution maps in medical records:
Launching the Pilot Program
To begin the project, the IT staff enabled the treatment planning computers in the radiation oncology department to send images to PACS.
Dr. Savjani and colleagues then configured their treatment software to include PACS as a Digital Imaging and Communications in Medicine (DICOM) location and to send images as a secondary capture DICOM structure set.
“This method takes each section in the desired plane exactly as it appears in our treatment software and compiles them into a composite single-standard DICOM file,” he said.
This DICOM file can then be uploaded to PACS and viewed by all health care providers, Dr. Savjani said.
“A dosimetrist, physicist or medical resident physician reviews the case after the completion of treatment for quality assurance and prepares the radiation therapy dose distribution map to upload to PACS,” Dr. Savjani said. “The dose map is never uploaded until after the patient has completed treatment, ensuring that planned or incorrect dose maps are not erroneously sent.”
After uploading to PACS, the volumes are retrieved in the PACS viewer and are inspected again to ensure the upload was successful. A treatment course can be added to PACS quickly — in approximately two minutes.
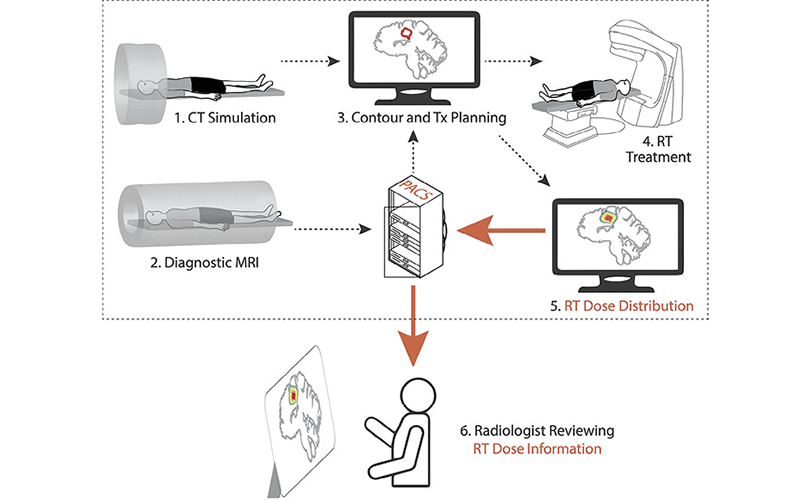
Connecting radiation oncology departmental computers to upload treatment plan images data into a picture archiving and communications system (PACS) enables sharing of radiation oncology–specific data with all medical providers. The radiation oncology workflow (top dotted box) includes obtaining diagnostic imaging and CT simulation scans, contouring and treatment planning, and the actual treatment delivery. This workflow largely remains as a black box to those outside of the field of radiation oncology. By exporting the radiation therapy (RT) dose distribution map to PACS (solid orange lines), the volumetric radiation history of a patient can be seen by radiologists for interpretation, by other oncologists for clinical evaluation, and in group settings such as tumor boards for multidisciplinary decision making.
Savjani et al, Radiology 2021 © RSNA 2021
Improving Communication and Encouraging Innovation
Sharing radiation dose distribution maps in PACS creates an opportunity for radiation oncologists and other medical providers who have less radiation oncology expertise to communicate with each other, Dr. Savjani said.
“But this is not a one-way stream,” he noted. “Our neuroradiologists have been educating us on how they radiographically differentiate effects of radiation changes versus progression, which is now made easier by having the dose information on the diagnostic studies.”
According to Dr. Savjani, making dose distribution maps easily accessible in PACS has simplified multidisciplinary meeting discussions.
“It has made discussions at our tumor board meetings faster and more productive,” Dr. Savjani said. “Now that everyone can see the new imaging and we can superimpose the old dose information, we can make our decisions more in real time, rather than having to dig through the data afterward.”
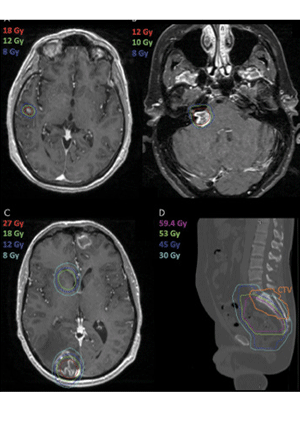
Isodose lines on a treatment planning MR image can be viewed on a picture archiving and communications system to allow radiologists and oncologists to readily know if a lesion received prior radiation treatment. Four example cases are shown in which the prior radiation dose aided in medical decision making. A, A previously treated lesion in the right superior temporal gyrus with SRS to 18 Gy 8 months prior showed residual enhancement at follow-up MRI. However, the new area of enhancement falls all within the 18-Gy isodose line, providing reassurance that the cause is likely radiation treatment effect. B, A right vestibular schwannoma was previously treated with 12 Gy at SRS 9 months prior with follow-up MR image now showing enhancement in the right cerebellopontine angle with increased size. The case was reviewed at our SRS conference, and consensus was made that the lesion shows radiation treatment effect given relation to prior isodose lines. C, A right occipital lesion was seen with enhancement after resection and postoperatively (SBRT) with 27 Gy to the resection cavity 12 months prior. The multidisciplinary team reviewed isodose lines without clear consensus whether the lesion represented treatment effect versus recurrence; consensus was made to try bevacizumab (Avastin) with possible reresection if no response. D, A previously treated colorectal adenocarcinoma to 59.4 Gy 3 years prior presented with sacral spine metastases. The CTV including S1-S3 was viewed on the CT simulation scan in relation to prior isodose lines, without significant prior overlap, giving confidence to proceed with 30 Gy in five fractions to the sacral spine. CTV = clinical target volume, SBRT = stereotactic body radiation therapy, SRS = stereotactic radiosurgery.
Savjani et al, Radiology 2021 ©RSNA 2021
In an accompanying Radiology: Imaging Cancer editorial, co-authors Shiv R. Khandelwal, MD, associate professor of radiation oncology and Sarah B. Scarboro, PhD, an assistant professor of radiation oncology, both at the University of Virginia School of Medicine, say that making radiation dose information available in PACS has the potential to improve imaging interpretation and management of oncology patients.
However, making this information readily available could, in some cases, increase the risk of misinterpretation of imaging findings and enhance the need for further education, according to Drs. Khandelwal and Scarboro.
“Given the need for diagnostic radiologists to also interpret radiation isodose maps accurately, perhaps there is a need to reintroduce a modest degree of formalized cross-training in radiology and radiation oncology residency programs,” the authors write.
For More Information
Access the Radiology: Imaging Cancer study, “A Framework for Sharing Radiation Dose Distribution Maps in the Electronic Medical Record for Improving Multidisciplinary Patient Management."
Access the accompanying Radiology: Imaging Cancer editorial, “Giving Radiologists and Other Clinicians the Tools to Identify Radiation Effects on Imaging Studies."
Read previous RSNA News articles on radiation dose:
- Report Shows Average Medical Radiation Doses in U.S. Are Decreasing
- Academic Pediatric Imaging Facilities Deliver the Lowest Radiation Dose