R&E Research Advances the Understanding of Acute Ischemic Stroke
Study demonstrates the effectiveness of non-contrast resting-state functional MRI


Neuroimaging is playing an increasingly critical role in the management and treatment of ischemic stroke, experts say.
“As the leading cause of disability and the fifth leading cause of death in the U.S., there is an urgent need to develop new ways to better treat ischemic stroke patients,” said Jeremy Heit, MD, PhD, an assistant professor of neuro-interventional radiology at Stanford University Medical Center.
In many ways, radiology is at the forefront of this effort.
“For example, neuroimaging plays a central role in both identifying patients who are eligible to receive endovascular thrombectomy (ET) and those most likely to benefit from the procedure,” Dr. Heit said.
Although this evaluation can be done using either CT or MRI, the best outcomes are achieved using perfusion weighted imaging (PWI). However, MR PWI requires gadolinium, which cannot be used in patients with impaired renal function — a major risk factor in stroke.
“This risk, combined with ongoing concerns about gadolinium deposition in the brain, means we need to develop new MRI methods for imaging the penumbra, which is at risk of dying from the stroke,” Dr. Heit said.
“If successful, these delay maps would allow stroke teams to identify the penumbra in a broader number of patients, including those with renal failure or gadolinium allergies.”
JEREMY HEIT, MD, PHD
Rs-fMRI an Attractive, Non-Contrast Alternative
According to Dr. Heit, one new method with such potential is non-contrast resting-state functional MRI (rs-fMRI), which was the subject of his 2016-2018 Bracco Diagnostics Inc./RSNA Research Scholar Grant, “Resting State Spontaneous Fluctuations of the BOLD Signal for Penumbra Assessment in Endovascular Stroke Candidates.”
Used in brain mapping, rs-fMRI evaluates the regional interactions that occur in a resting state. These resting state conditions are observed through changes in blood flow to the brain, which creates a blood-oxygen-level dependent (BOLD) signal that can be measured using fMRI.
“Resting state functional MRI delay maps show promise for identifying impaired brain flow in patients with chronic forms of cerebral ischemia,” Dr. Heit said. “And, because it doesn’t require gadolinium and can be performed in just minutes, it is an attractive alternative to perfusion-weighted imaging.”
In his RSNA-funded research, Dr. Heit investigated the utility of using rs-fMRI to evaluate the eligibility of an ischemic stroke patient for endovascular treatment. The study included 124 patients with acute ischemic stroke caused by a large vessel occlusion (AIS-LVO) who underwent MRI triage for ET.
Dr. Heit and colleagues performed diffusion-weighted imaging, gradient-echo, time-of-flight MR angiography, rs-fMRI, and MR perfusion sequences on all patients. ET treatment decisions were made based on the clinical and standard of care imaging evaluation of patients issued by the U.S. Preventative Services Task Force.
Next, rs-fMRI sequences were processed and used to generate delay maps. All imaging was then blindly reviewed to determine whether rs-fMRI generated delay maps could identify salvageable penumbra at the same level as that achieved using MR perfusion time-to-maximum (Tmax) maps.
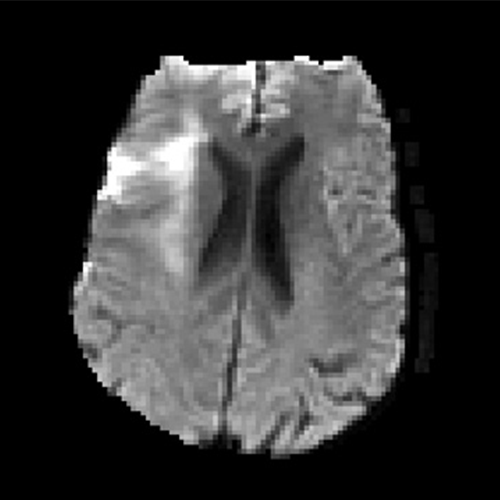
Determining that rs-fMRI delay maps have the potential to serve as an equivalent alternative to standard MR perfusion maps is a key finding of his research, Dr. Heit said.
“If successful, these delay maps would allow stroke teams to identify the penumbra in a broader number of patients, including those with renal failure or gadolinium allergies,” Dr. Heit said. “It is also possible that rs-fMRI delay maps may provide additional prognostic information for stroke patients, but further studies are needed.”
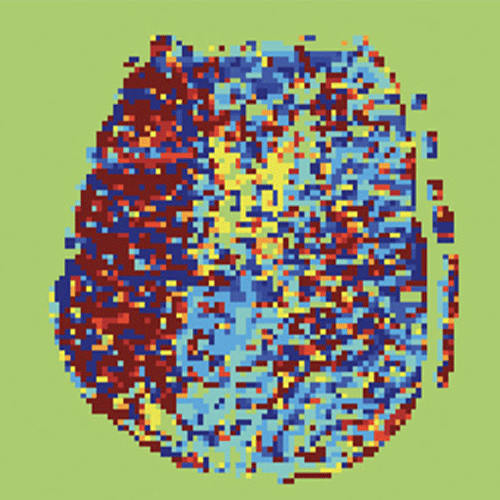
Nevertheless, the use of rs-fMRI with ischemic stroke patients does have limitations.
“We quickly learned that rs-fMRI delay maps are very sensitive to patient motion,” Dr. Heit said. “Unfortunately, the nature of the stroke makes it extremely difficult to prevent these patients from moving.”
Currently, Dr. Heit is exploring whether motion correction techniques or artificial intelligence (AI) processing approaches can potentially alleviate this shortcoming, opening the door to wider use of rs-fMRI.
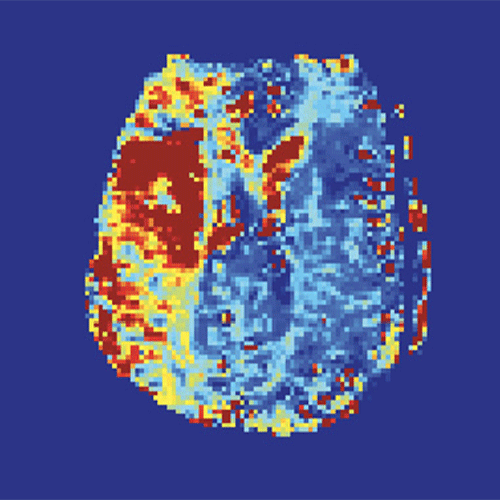
Dr. Heit is confident his ongoing research will not only advance the understanding of acute ischemic stroke, but also improve the utility of imaging for ischemic stroke patients.
“Stroke is such an important issue, and treating it really starts with the imaging, which is why research conducted through the RSNA grant I was awarded is so essential,” Dr. Heit said. “The grant has provided critical support and guidance as I move toward becoming an independent investigator.”
And the grant opened the door to subsequent stroke research. For example, Dr. Heit participated in an RSNA 2020 Hot Topic session, where he discussed how the recent publication of five randomized trials (MR CLEAN, REVASCAT, ESCAPE, SWIFT PRIME, and EXTEND-IA) has led to a significant increase in the use of thrombectomy.
With the right motion correction techniques, the R&E study will set the stage for a larger prospective study, ideally with funding from the National Institutes of Health, Dr. Heit said.
“I’m excited about the potential that this technology has as an imaging selection and prognostic tool that can be used to improve the way we treat acute ischemic stroke,” he said.
For More Information
Access the RSNA 2020 Hot Topic session, “Stroke Imaging – How Recent Trials Are Changing Radiologists’ Practices,” at RSNA2020.RSNA.org.
Learn more about R&E Foundation funding opportunities.
Connect with Dr. Heit @JeremyHeitMDPHD
Read previous RSNA News articles on ischemic stroke: