Liquid Biopsy Emerges as Powerful Tool in Cancer Care
Noninvasive diagnostic technique is poised to bring change to radiology


Liquid biopsy — a novel and fast-evolving, non-invasive technique in cancer diagnosis and care — is emerging as a revolutionary tool that will present new challenges and opportunities for radiology, according to a recent Radiology review.
By reducing the need for image-guided biopsies, liquid biopsy has the potential to have a disruptive impact on radiology. But the technique also stands to complement radiology by playing a guiding role in determining when to image and how to interpret imaging findings, the authors say. Liquid biopsies are tests conducted on blood samples that examine biomarkers shed by tumors, such as cancer cells or pieces of tumor DNA.
“The presence of circulating tumor cells has been known for over a century and has been more frequently studied over the last decade. In addition, with the inclusion of circulating tumor DNA over the last few years, the number of research papers on the subject has increased tremendously and the enthusiasm of oncology community has really grown,” said the review’s senior author, Patrick Sutphin, MD, PhD, an interventional radiologist at Massachusetts General Hospital in Boston.
“One of the big benefits I see with liquid biopsy is the ability to monitor a cancer patient’s blood for mutations that might lead to resistance to the medication that they are on."
PATRICK SUTPHIN, MD, PHD
“I think liquid biopsy will be less anxiety-provoking for the patient and less resource-intensive than tissue biopsy and could be performed on a more frequent basis,” Dr. Sutphin said.
On the diagnostic side, liquid biopsies can provide crucial information on genetic mutations in tumors that may help guide treatment.
“It can be really helpful to have ongoing information on how a tumor is evolving and changing in response to treatment, but it’s not always feasible to do a lot of tissue biopsies during a treatment course,” said the review’s first author, Jacob Underwood, DO, of the Spokane Teaching Health Center, Spokane, Wash. “Liquid biopsy typically just involves drawing blood. We can do it much more regularly, which can be helpful in between tissue biopsy or in between times when repeat imaging is necessary.”
Numerous Roles in Cancer Care
Existing research points to several roles for liquid biopsy in cancer care. Along with tracking tumor changes, the technique could also help predict response to treatment. Mutations found in the tumor’s genetic code could be used to decide which patients would benefit from a specific therapy option.
“One of the big benefits I see with liquid biopsy is the ability to monitor a cancer patient’s blood for mutations that might lead to resistance to the medication that they are on,” Dr. Sutphin said. “Ideally, through a simple blood draw, we will be able to either capture the tumor cells themselves or portions of the tumor cells, particularly the circulating tumor DNA that can be evaluated through sequencing to enlighten us on the characteristics of that tumor.”
“Medicine is moving away from a one-size-fits-all approach and looking more at individual variability in genes and environmental factors, particularly for cancer,” Dr. Underwood added. “Knowing the mutations that a tumor has or doesn’t have is really helpful for knowing the metastatic potential of the cancer and how responsive it will be to different types of treatment.”
Potential for Disruption
Because it could displace some imaging exams, liquid biopsy looms as a potentially disruptive force in radiology. There is also speculation that it could replace tissue sampling in some circumstances. In the near term, the review authors see it playing a complementary role to imaging. For instance, liquid biopsy could serve a complementary role to screening mammography. A patient could have screening mammography and a blood test that looks for specific markers seen in breast cancer.
The findings would then be used in conjunction to guide decisions about additional breast imaging, either through diagnostic mammography, ultrasound or MRI as well as help guide decisions on biopsy to reduce the number of excessive biopsies. On the interventional side, liquid biopsy could show certain mutations in tumors that might make them more susceptible to treatments like radioembolization or cryoablation.
“It’s possible that as liquid biopsy develops, imaging for screening is going to be less utilized,” Dr. Underwood said. “But more cancers will be detected if liquid biopsy is widely adopted, so we will need to follow up with imaging to figure out exactly where the cancer is and its anatomical stage.”
While the technique does have limitations and more clinical data is needed, liquid biopsy is clearly attracting significant attention from researchers and industry. Radiologists would be well-advised to prepare for its arrival in the clinic, the authors said.
“In writing this paper, we hope to start a discussion on how liquid biopsy will impact medical imaging so that radiologists can not only be better prepared for how to respond to the changes it could bring, but also be ready to take advantage of opportunities to utilize the technology,” Dr. Underwood said. “Radiologists should also be involved in developing any screening protocols that utilize both liquid biopsy and imaging in parallel.”
For More Information
Access the Radiology Review and Commentary, “Liquid Biopsy for Cancer: Review and Implications for the Radiologist.”
Access a podcast on the review by Radiology Editor David Bluemke, MD, PhD, at RSNA.org/Radiology.
Access an RSNA online education course related to this Radiology article at RSNA.org/Learning-Center.
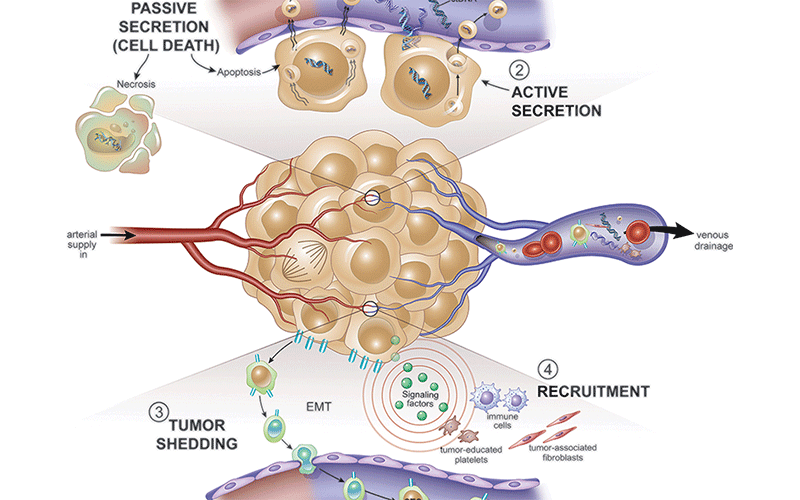
Illustration shows mechanisms of translocation of tumor cells and cellular components into bloodstream. Noncellular tumor components may enter bloodstream through (1) passive secretion during cell death by apoptosis or necrosis or (2) active secretion. (3) Epithelial-mesenchymal transition leads to enhanced ability for tumor cells to migrate. (4) Recruitment from native tissues also contributes to release of these cells and factors into bloodstream. cfRNA = cell-free RNA, CTC = circulating tumor cell, ctDNA = circulating tumor DNA, EMT = epithelial-to-mesenchymal transition cell.
Underwood, et al, Radiology 2020 ©RSNA 2020