COVID-19 Sparks Innovations in Radiology Departments
COVID SWAT team among novel solutions to aid patients during pandemic
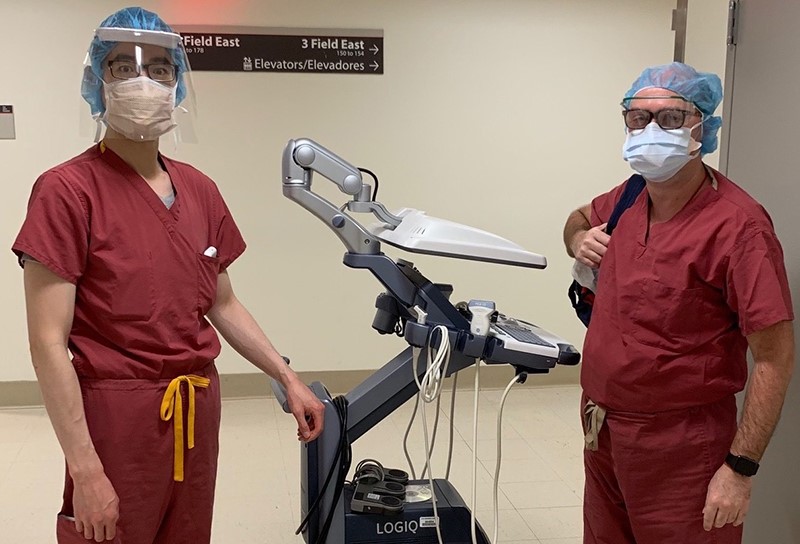
Vladimir Sheynzon, MD, (left), and resident David Xu, MD, en route to the ER at Allen Hospital in New York to place lines in patients’ veins and arteries. Dr. Sheynzon and a team of residents served on the Surgical Workforce Access Team, or COVID SWAT for short, that aided patients during the COVID-19 pandemic. Image courtesy of NewYork Presbyterian Hospital.



Vladimir Sheynzon, MD, arrived at NewYork Presbyterian Allen Hospital in Manhattan in late March to an alarming scene. Patients, many in serious condition with symptoms of COVID-19, lined the corridors all the way to the elevators. The view of the ambulance bay from Dr. Sheynzon’s second-floor office reflected the desperate circumstances.
“Normally, you see one ambulance coming in every 20 minutes or so, but on those days, they were lined up on the driveway coming into the emergency room,” he recalled. “Three or four ambulances would unload patients and leave, then another three or four would come in to take their place.”
Dr. Sheynzon, an interventional radiologist at Columbia University Medical Center and NewYork Presbyterian, had come to Allen Hospital as part of a Surgical Workforce Access Team, or COVID SWAT for short. He and his team of resident physicians were there to perform the difficult but important job of placing lines into patients’ veins and arteries to deliver fluids and medications. The work was sorely needed, as the hospital’s surgeons were swamped with patients and most of the other physician specialists who were pitching in to help had only limited experience placing lines.
“It would be nearly impossible for someone who hasn’t touched a needle in a long time to place these lines,” Dr. Sheynzon said. “Asking these physicians to do that plus making all the clinical decisions would have been overwhelming.”
Using ultrasound for guidance, the SWAT teams from the Departments of Radiology and Surgery worked around the clock, running lines into the very small radial arteries in the wrist for some patients and placing large catheters in the necks of others who were undergoing dialysis.
Staff worked at considerable personal risk and sacrifice. Dr. Sheynzon and his physician wife sent their children to live with their grandparents until the pandemic abated in mid-May.
“It was incredibly sad to see all those patients, but it was inspiring the way this institution was able to convert all the operating rooms to a COVID ICU,” he said. “Otherwise, we would have run out of room. We were able to save so many people.”
Radiology Annex Aids Patient Volume
The pandemic challenged radiology departments across the country to maintain efficiency under extraordinary circumstances, often resulting in innovative solutions. For example, the staff at Penn State Health in Hershey, PA, opened a new Radiology Annex just as the number of COVID-19 cases was nearing its peak.
Intermediate-risk patients with COVID-19 symptoms were coming in to get chest X-rays to rule out other conditions, potentially exposing the staff and other patients to the virus. In addition, rooms had to be decontaminated after each patient, a time-consuming process that limited the number of patients examined. One of the technologists then came up with a novel idea: Perform the X-rays without ever having the patient enter the room.
Staff at the ambulatory site found an area with an exterior-facing door where they positioned a sheet of plexiglass, creating a secure barrier between the machine and the outdoors. Patients getting an X-ray only had to drive up, get out of their car and stand in front of the plexiglass.
“A technologist stood outside to greet the patient, walk them over and get them positioned, but they were completely isolated from any other patient so there was no cross-exposure and no potential contamination with the instruments,” said Timothy J. Mosher, MD, the Kenneth L. Miller Chair and Distinguished Professor, Department of Radiology, Penn State University College of Medicine in Hershey.
Within days of opening, the facility was seeing up to 15 cases a day, more than twice the volume possible in a room under airborne decontamination procedures.
“It turned out to be a very effective way of handling large volumes,” Dr. Mosher said. “From a patient flow standpoint, it was extremely convenient, and we didn’t have to take a room down, so we were able to maintain a high level of capacity.”

Predictive Tool Tests for COVID-19
The pandemic’s rapid advance exposed limitations in the measures used to predict future cases, leaving many communities with a shortage of personal protective equipment, hospital beds and staff. These limitations inspired Lawrence “Rusty” Hofmann, MD, professor and chief of interventional radiology at Stanford University School of Medicine, CA, to develop a better predictive tool through an online survey.
By inviting participants to give daily updates on their condition, the survey functions as a sort of digital version of the physical swab used to test for the virus. Information is used in tandem with local test results to predict surges by region.
“A physical swab represents one point in time,” Dr. Hofmann said. “You can get infected as soon as you leave the testing center. This survey, by contrast, tests the population continuously.”
The survey begins by asking participants to fill in demographic information like their zip code, age, gender and if they are experiencing any “COVID-like” symptoms. Participants then check in every day and note whether their condition is better, worse or the same.
“That’s the real power of this,” Dr. Hofmann said. “If people take the survey every single day, we believe we only need 1,000 to 2,000 people per county to make this work, and then we’ll be able to get seven-to-10 days advance notice on what’s going on in a community.”
The site has had millions of visits thanks in part to the help of T-Mobile, the social site Nextdoor.com and a California-based company, EZ Texting that is providing daily SMS reminders. Currently, the survey is only available in the U.S., but Dr. Hofmann hopes to expand it internationally in the near future.
Long-term Impact
COVID-19-inspired innovations like those at Stanford and Penn State will probably remain in some form long after the pandemic is over. Likely to endure even longer are the inspiring stories of health care workers who braved difficult conditions to help the thousands of patients affected by the virus.
“It was remarkable to see so many people going in and taking care of the patients even though there was a high concentration of COVID-19 in the hospital,” Dr. Sheynzon said. “I was very proud of the way that they all stepped up.”
For More Information
Access the Stanford University online survey.
Access RSNA's full roster of COVID-19 resources.
Read additional RSNA News stories about ways radiologist's have stepped up during the COVID-19 pandemic, including, Radiology Answers the Call During COVID-19 Pandemic and Radiology Trainees on the Front Lines of COVID-19.