Supplemental MRI Beneficial for Women with Extremely Dense Breasts
DENSE trial shows MRI can improve cancer detection


Note: This story is part of an RSNA Special Focus section on breast cancer screening. The other two stories are listed below.
Although screening mammography is the primary modality for detection of breast cancer, it may not be as accurate for women with dense breasts, sometimes leading to false positives that can be expensive and stressful.
However, new research recently published in Radiology details the effectiveness of adding MRI, a more sensitive screening tool, for these women.
DENSE (The Dense Tissue and Early Breast Neoplasm Screening), is a prospective multicenter trial embedded within the Dutch population-based biennial digital mammography screening program for women between 50 and 75 years old. Women were eligible for the DENSE trial if they had a negative mammography result and extremely dense breast tissue. Trial participants were randomized to the intervention arm (invitation to undergo supplemental MRI screening), or to the control arm (biennial mammographic screening).
Second round results showed that the cancer detection was 5.8 per 1,000 screenings, compared to a cancer detection rate of 16.5 per 1,000 in the first round. The false positive rate was sharply reduced from 79.8 per 1,000 screening examinations in the first round to 26.3 per 1,000 screening examinations in the second round.
“This research is very important as we know that women with dense breasts have a higher breast cancer risk and because the density of their breast tissue makes it more difficult to detect breast cancers with mammography,” said Stefanie Veenhuizen, a PhD student at the Julius Center for Health Sciences and Primary Care, University Medical Center, Utrecht, the Netherlands, and study lead author.
Women with dense breasts also tend to have a higher risk of interval cancers (cancers diagnosed in between screening rounds), she explained, adding that previous research showed supplemental MRI screening can significantly reduce that risk. “It is reassuring to see that the false-positive rate sharply decreases in incident screening rounds, and that still a significant number of breast cancers are detected with MRI,” Veenhuizen said.
Linda Moy, MD, professor of radiology at New York University’s Grossman School of Medicine and senior deputy editor with Radiology, said she was encouraged by the results. Dr. Moy authored an editorial that accompanied the Radiology article.
Watch Dr. Moy discuss the DENSE trial and its importance for women with dense breasts:
In the editorial she notes that compared to women with fatty breasts, women with extremely dense breasts are 17.8 times more likely to have interval cancers after a negative mammogram. The interval cancer rate has become a powerful indicator of the robustness of a screening tool.
“It is therefore highly promising that the interval cancer rate was reduced by more than half in women with extremely dense breasts who underwent supplemental MRI in the prevalence screening round of the DENSE trial,” Dr. Moy said.
The trial’s early detection of small, node-negative invasive cancers of good prognosis is also clinically important, Dr. Moy said, especially in women with extremely dense breasts where mammographic sensitivity is limited. However, she noted, further screening and data need to be collected to find if ongoing supplemental MRI screening in this population will improve mortality.
Most promising, Dr. Moy said, was the reduction in false positive test results. “False positive findings lead to anxiety with additional follow up exams and biopsies, as well as additional cost to the health care system,” she said.
While the results from the DENSE study are encouraging, Dr. Moy said it was surprising that only 59% of women accepted the invitation to have a supplemental MRI, which shows the need for further education and acceptance of MRI as a modality for breast cancer screening in addition to mammography. “We need to figure out why women were reluctant to have the test,” Dr. Moy said, speculating that it could be cost or lack of education about MRI benefits among patients and providers.
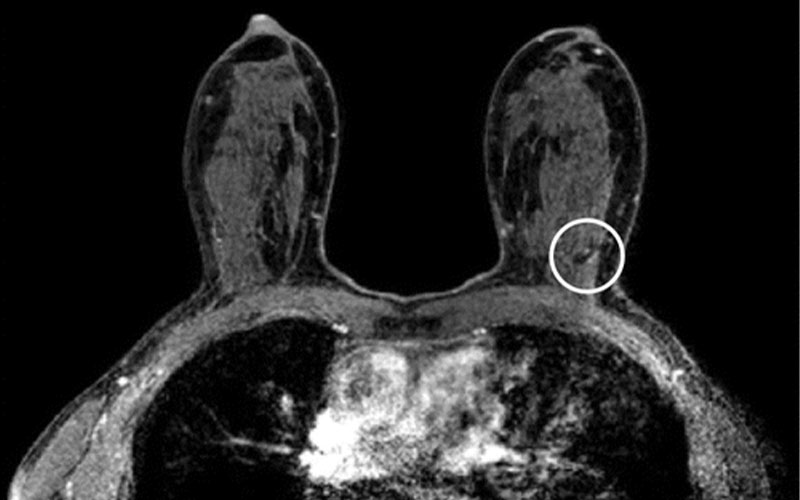
MRI scans in a 54-year-old participant in the second round compared with (c) the MRI scan from the first round (prevalence round). Her current axial post-contrast T1-weighted MRI scan (a) shows a sharply demarcated 3-mm lesion in the left upper outer quadrant (arrow). The lesion shows type 2 kinetics (kinetic overlay not shown) and no diffusion restriction (circled area on b) on the axial apparent diffusion coefficient map (b). In a non–high-risk screening examination, this indifferent focus would normally not be recalled. In this case, the participant was recalled because comparison with her prior axial post-contrast T1-weighted MRI scan (c) revealed that this focus was new (circled area on c). Biopsy showed an infiltrating lobular carcinoma.
Veenhuizen et al, Radiology 2021; 299:278–286; © RSNA 2021
Researchers said the data can also be used to specialize screening programs based on a woman’s needs.
“For the health professionals it is important to realize that not all women may benefit from the same breast cancer screening program, depending on their risk and breast tissue structure,” Veenhuizen said. “There is now evidence that MRI screening is effective in women with extremely dense breast tissue, and that the risk of false-positives strongly decreases after the first MRI.”
For More Information
Access the Radiology study, “Supplemental Breast MRI for Women with Extremely Dense Breasts: Results of the Second Screening Round of the DENSE Trial.”
Read the accompanying Radiology editorial, “Supplemental MRI in Extremely Dense Breasts: Sharp Reduction in False-Positive Rate in the Second Screening Round of the DENSE Trial.”
Read previous RSNA News stories on breast imaging: