Using Radiomic Features from Mammography to Predict Upstaging of DCIS
Ability to predict invasive cancer or DCIS could help patients choose optimal treatment strategy



Ductal carcinoma in situ (DCIS) is a non- or pre-invasive form of breast cancer that accounts for nearly 15% of all new breast cancer diagnoses. While DCIS itself is not life-threatening—for many it never progresses to invasive cancer—it is a precursor to invasive ductal carcinoma.
“The standard of care is that everyone with DCIS has it surgically removed, regardless of whether or not invasive cancer is present,” said Lars Grimm, MD, breast imager and associate professor of radiology at Duke University Medical Center, Durham, NC. “But we’re starting to recognize that a lot of women are being over treated as the condition may never progress or impact their lives.”
“Fewer than half the DCIS cases become invasive, yet we still treat it like full-blown cancer,” added Joseph Lo, PhD, professor of radiology and vice chair for research of radiology at Duke University Medical Center. “The challenge is figuring out which DCIS cases can forgo treatment without risking delayed detection of invasive cancer.”
One potential solution for striking this balance between overtreatment and delayed detection is active surveillance. However, a prerequisite for doing active surveillance is having the ability to predict who has invasive cancer and who has pure DCIS.
“Being able to do this would have important clinical implications and assist both physicians and patients in choosing optimal management strategies,” Dr. Grimm said.
A Very Large and Thorough Dataset
Using digitally extracted mammographic radiomic features, in conjunction with traditional clinical features, Drs. Grimm, Lo and their colleagues investigated whether a radiomics approach could predict occult invasive cancer among women diagnosed with DCIS on the basis of core biopsy findings. The study was published in Radiology.
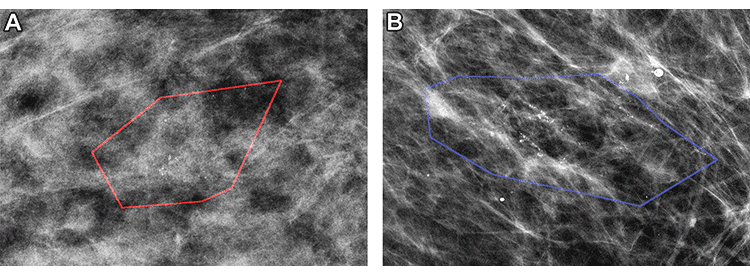
Mammographic images of patients with biopsy-proven ductal carcinoma in situ (DCIS). (A) A 55-year-old woman (right magnification craniocaudal view) diagnosed with DCIS only; model correctly classified as negative findings. (B) A 64-year-old woman (left magnification mediolateral oblique view) with DCIS at core biopsy but subsequently upstaged to invasive disease; model correctly classified as positive findings. Red and blue polygons show lesions annotated by the radiologist.
Hou et al, Radiology 2022; 303:54–62 ©RSNA 2022
“Whereas most AI-related work tends to focus on general screening, our study is unique in that it attempts to use AI for a very specific task,” Dr. Grimm explained.
Specifically, the study assessed the performance and clinical utility of mammographic radiomic features in predicting occult invasive cancer among women diagnosed with DCIS on the basis of core biopsy findings. Furthermore, the research focused on the more challenging subset of women with DCIS who presented only with calcifications, because these women could be eligible for active surveillance.
“When creating models specifically for active surveillance, you have to make sure you don’t miss any invasive cancer,” said Rui Hou, PhD, postdoctoral associate in the departments of radiology and of electrical and computer engineering at Duke University Medical Center and the study’s lead author. “Not only does this require very high sensitivity, it also requires creating a very large and thorough dataset.”
“With more data, we’ll be able to refine our tools and really be able to see whether we can make it safe for women to do active surveillance. As we add more markers, enhance our models and refine our databases, we’ll get to the point where we can have a meaningful clinical impact on our patients and how we select who may or may not benefit from active surveillance, and who may require surgical excision.”
— RUI HOU, PHD
During her dissertation research, Dr. Hou spent five years preparing the dataset, which consisted of mammograms from 700 women with asymptomatic DCIS.
Demonstrating the Value of Radiomics
Ultimately, the study demonstrated that radiomic features from mammography, particularly when combined with clinical features, have the potential to predict upstaging of DCIS.
“As a proof of concept, this work shows the value of using radiomics for a specific clinical task,” Dr. Grimm noted.
“Our research is the first to use data to define which DCIS cases are less or more likely to become invasive cancer,” Dr. Lo added. “Having this capability will help physicians and their patients make more informed decisions about their treatment plans.”
The research team is now working to test its models against larger datasets, including such data as additional biomarkers, demographics and imaging modalities.
“With more data, we’ll be able to refine our tools and really see whether we can make it safe for women to do active surveillance,” Dr. Hou concluded. “As we add more markers, enhance our models and refine our databases, we’ll get to the point where we can have a meaningful clinical impact on our patients and how we select who may or may not benefit from active surveillance, and who may require surgical excision.”
For More Information
Access the Radiology study, “Prediction of Upstaging in Ductal Carcinoma in Situ Based on Mammographic Radiomic Features.”
Read previous RSNA News stories about breast cancer:
- Machine Learning May Inform Patients’ Eligibility for Breast Cancer Clinical Trials
- Big Data Advances Ability to Automatically Segment Breast Tumors
- Six-Month Follow-Up Appropriate for BI-RADS 3 Findings on Mammography