Radiology Plays Vital Role in Detecting Intimate Partner Violence
Research shows medical imaging can offer early clues of domestic abuse




As residents, radiologists learn early on about telltale signs of non-accidental trauma in children, and emerging research is helping more radiologists identify victims of elder abuse. Although one in four women has reported experiencing intimate partner violence (IPV) in their lifetime in the U.S., there has been little research correlating imaging findings with abuse by a current or former partner or spouse.
A recent study in Radiology is beginning to change that. The study’s principal investigator, Bharti Khurana, MD, director of emergency musculoskeletal radiology at Brigham and Women’s Hospital and assistant professor of radiology at Harvard Medical School, both in Boston, was inspired by the case of a young woman whose head CT showed an acute nasal bone fracture superimposed on an older healed nasal bone fracture.
While reviewing the patient’s prior studies, Dr. Khurana also noticed a recent wrist fracture, which raised suspicion that the woman was a victim of domestic violence. While Dr. Khurana did not pursue the matter further, the case stuck with her. A month later during a trauma “hackathon” — a gathering of health care providers collaborating on software projects — she learned that physicians frequently miss the signs of intimate partner violence.
Dr. Khurana immediately decided to conduct a study seeking to define injury patterns seen in intimate partner violence victims. She connected with colleagues at Brigham already working on the clinical and social aspects of intimate partner violence and inspired three radiology residents to collaborate on this under- explored topic for the Radiology study, “Radiologic Findings in Intimate Partner Violence.”
By assessing the “entire clinical picture”— including sociodemographic and economic factors — along with radiology findings, the team began piecing together a portrait of a patient at risk for intimate partner violence.
Eventually, this line of inquiry could lead to an algorithm for detecting intimate partner violence that is similar to one that currently exists for detecting child abuse. “Already, the results could both raise awareness of this public health problem among radiologists and encourage them to look at findings in a new light,” said Elizabeth George, MD, first author of the study, a former resident at Brigham and now a fellow in neuroradiology at the University of California, San Francisco.
“Radiology has an important role in the discovery of these patients and in potentially saving their lives,” said Efren Flores, MD, officer, Radiology Community Health & Equity and a radiologist, Thoracic & Emergency Divisions, Massachusetts General Hospital (MGH), who wrote an accompanying editorial in Radiology.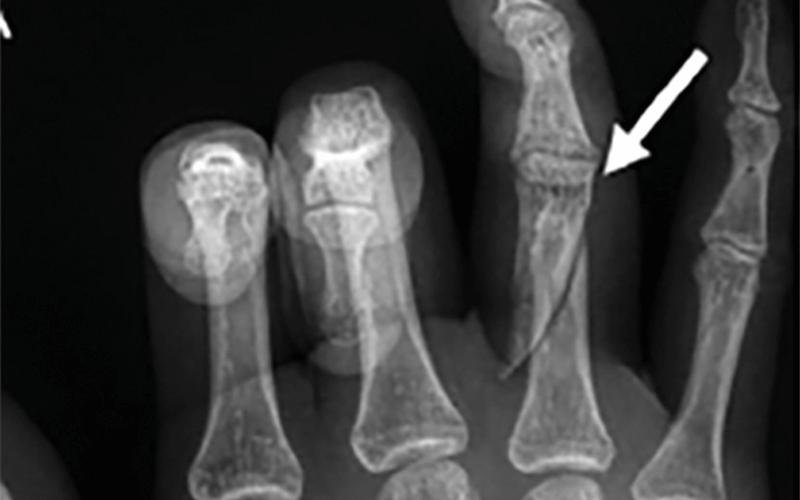
Understanding the Full Picture
In the Radiology study, researchers studied the records of 185 emergency department (ED) patients who reported intimate partner violence and were referred to the BWH support program between January 2015 and October 2016. They compared these patients to a control group of 555 patients seen in the ED. One of the most striking elements of the results, Dr. George said, was that in the five years prior, victims of intimate partner violence underwent imaging about four times more often than the general population.
“Victims of abuse are accessing healthcare and undergoing imaging studies,” Dr. George said. “Radiologists need to be more cognizant of this diagnosis, be aware of the imaging findings, and work towards being able to identify these patients early.”
The study results offer radiologists clues as to exactly what to watch for. Acute fractures and obstetric/gynecologic complications — for instance, pregnancy loss and intrauterine growth restriction — were associated with greater odds of intimate partner violence.
Almost all the victims — 96% — were women, and most were non-white (37% African American and 28% Hispanic). They were also more likely than control patients to be homeless, have a history of psychiatric disorders, or have a substance use disorder.
Particularly alarming, Dr. George said, was the frequency of strangulation. About one in four victims of intimate partner violence reported a history of the violent act. The strong association between strangulation and future homicide risk underscores the importance of identifying victims before it’s too late.
One Question Helps Identify Victims
The sheer volume of patients and the nature of the work puts radiologists in a prime position to spot these troubling signs and make a difference in victims’ lives.
Any type of health care visit can open the door to a conversation about abuse. Breast imaging, specifically, lends itself to identification and intervention of this issue due to its intimate nature and widespread access. After all, the majority of women 40 and older undergo screening for breast cancer, noted Anand K. Narayan, MD, PhD, assistant professor of radiology at MGH.
The approach taken by Constance D. Lehman, MD, PhD, professor of radiology at MGH, Dr. Narayan and colleagues at the hospital is to add a single question to intake forms to screen for intimate partner violence: “Do you feel safe at home?” If a woman screens positive, she’s referred to services through the institution’s Help Abuse and Violence End Now (HAVEN) program, he said.
Dr. Narayan is the first author of a study in the April 2019 Journal of the American College of Radiology demonstrating the feasibility of this system in radiology departments.
“When victims connect with anybody in the health care system, we want to make them feel safe, that we’re not here to pass any judgment, and that our main priority is to take care of them,” Dr. Flores, a co-author on the study, said.
Empowering Physicians with Artificial Intelligence (AI)
Long-term, Drs. Lehman, Narayan and Khurana plan to use AI to analyze images and other data, including information from medical records. The end goal is creating an AI-powered system that automatically detects high-risk patterns and alerts clinicians.
Still, radiologists don’t have to wait to act, Dr. George said. We should ask ourselves whether the imaging findings we are assessing could signal intimate partner violence in the appropriate clinical scenario and bring suspicions to the referring physician. Radiologists can also connect patients with resources in and outside of their institutions.
“Our pilot study has allowed us to create an exhaustive list of imaging and clinical findings that are associated with intimate partner violence. However, radiologists often do not have enough time to access and assimilate all available information, especially in acute settings,” Dr. Khurana said. “Therefore, we are now developing an integrated, multi-dimensional clinical decision support tool based on patterns derived from expert analysis of historical radiological and clinical data.”
Dr. Khurana and fellow researchers are working with clinical colleagues in orthopedic surgery, emergency medicine, primary care, women’s health and plastic surgery at Brigham, MGH, Boston Medical Center, Harvard Medical School, Ariadne Labs, and Harvard T.H. Chan School of Public Health to classify injuries likely stemming from intimate partner violence and to create an automated alert system.
According to Dr. Khurana, AI will play an increasingly significant role in identifying domestic violence. She credits her Brigham mentors, Steven Seltzer, MD, chairman emeritus, and Giles Boland, MD, chairman, with encouraging the integration of AI into her Radiology study.
Dr. Khurana is continuing her research on intimate partner violence through a prestigious Innovation Discovery Grant and is in the process of applying for extramural funding. She will present a session on this topic at RSNA 2019.
For More Information
Access the study, “Radiologic Findings in Intimate PartnerViolence,” and the accompanying editorial, “The Role of Radiology in IntimatePartner Violence,” at RSNA.org/Radiology.
Access the study, “Implementation of an Intimate Partner Violence Screening Assessment and Referral System in an Academic Women’s Imaging Department,” at JACR.org.